An Expert’s Perspective on Advanced Non-Melanoma Skin Cancer Research
An Expert’s Perspective on Advanced Non-Melanoma Skin Cancer Research from Patient Empowerment Network on Vimeo.
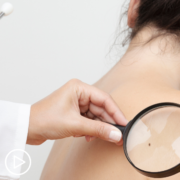
What’s the latest in advanced non-melanoma skin cancer research? Dr. Sunandana Chandra shares an update on emerging treatments and provides reliable resources for research news.
Dr. Sunandana Chandra is a medical oncologist and Associate Professor of Medicine at Robert H. Lurie Comprehensive Cancer Center of Northwestern University. Learn more about Dr. Chandra.
Related Resources:

What Are Treatment Goals and Considerations for Advanced Non-Melanoma Skin Cancer? |
A Review of Current Advanced Non-Melanoma Skin Cancer Treatment Options |

|
Transcript:
Katherine:
Are there developments in advanced non-melanoma skin cancer treatment and research that patients should know about?
Dr. Chandra:
So, you know, in the past, as a medical oncologist, we used to use a lot of chemotherapy.
So, these are drugs that are notoriously hard to tolerate. Patients, understandably, are fearful of them and many of them don’t want them. They’ve seen friends and family go through them. And frankly, they have not been the most effective or efficacious in treating non-melanoma skin cancers, traditionally. But in the past, that’s all we had.
Now, we actually have much better therapies, specifically, the category of drugs called immunotherapy drugs that really boost a person’s own immune system to fight the cancer. These drugs are fairly new in the cancer world, and certainly new in the non-melanoma skin cancer world, and so, many of our colleagues in the community may not necessarily think of them when they’re considering patients.
Perhaps, a lot of our patients haven’t even gotten a chance to hear about them. So, yes. There are new developments that I think are worth considering earlier and earlier in the course of a person’s treatment course. And so, I think an earlier referral to these multidisciplinary team members, including a medical oncologist, may not be a bad idea.
Katherine:
How can patients stay up-to-date on developing research? What’s available for them?
Dr. Chandra:
So, you know there are skin cancer patient advocacy websites that they can check out, skincancer.org. I always tell patients to be careful about what website they’re checking, because I certainly want them to go to a website that’s reputable, that’s vetted, that is something that we think has accurate information that’s evidence-based.
And so, AIM at Melanoma has a non-melanoma skin cancer educational website. It’s called SCERF, which is Skin Cancer Education and Research Foundation, and you can find that through the aimatmelanoma.org website. You can look at skincancers.org, you can try with American Cancer Society, or you can even ask your clinical care team and see if they have any suggestions. There’s a lot of resources out there. I would just urge our patients to be careful in what source they’re looking at just make sure that they’re getting accurate, evidence-based information.