Most melanomas are brought to a doctor’s attention because of signs or symptoms a person is having.
If you have an abnormal area on your skin that might be cancer, your doctor will examine it and might do tests to find out if it is melanoma, another type of skin cancer, or some other skin condition. If melanoma is found, other tests may be done to find out if it has spread to other areas of the body.
Medical history and physical exam
Usually the first step your doctor takes is to ask about your symptoms, such as when the mark on the skin first appeared, if it has changed in size or appearance, and if it has been painful, itchy, or bleeding. You may also be asked about your possible risk factors for melanoma skin cancer, such as your history of tanning and sunburns, and if you or anyone in your family has had melanoma or other skin cancers.
During the physical exam, your doctor will note the size, shape, color, and texture of the area(s) in question, and whether it is bleeding, oozing, or crusting. The rest of your body may be checked for moles and other spots that could be related to skin cancer (or other skin conditions).
The doctor may also feel the lymph nodes (small, bean-sized collections of immune cells) under the skin in the neck, underarm, or groin near the abnormal area. When melanoma spreads, it often goes to nearby lymph nodes first, making them larger.
If you are being seen by your primary doctor and melanoma is suspected, you may be referred to a dermatologist, a doctor who specializes in skin diseases, who will look at the area more closely.
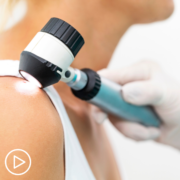
Along with a standard physical exam, many dermatologists use a technique called dermoscopy (also known as dermatoscopy, epiluminescence microscopy [ELM], or surface microscopy) to see spots on the skin more clearly. The doctor uses a dermatoscope, which is a special magnifying lens and light source held near the skin. Sometimes a thin layer of alcohol or oil is used with this instrument. The doctor may take a digital photo of the spot.
Skin biopsy
If the doctor thinks a spot might be a melanoma, the suspicious area will be removed and sent to a lab to be looked at under a microscope. This is called a skin biopsy.
There are many ways to do a skin biopsy. The doctor will choose one based on the size of the affected area, where it is on your body, and other factors. Any biopsy is likely to leave at least a small scar. Different methods can result in different types of scars, so ask your doctor about scarring before the biopsy. No matter which type of biopsy is done, it should remove as much of the suspected area as possible so that an accurate diagnosis can be made.
Skin biopsies are done using a local anesthetic (numbing medicine), which is injected into the area with a very small needle. You will likely feel a small prick and a little stinging as the medicine is injected, but you should not feel any pain during the biopsy.
Shave (tangential) biopsy
For this type of biopsy, the doctor shaves off the top layers of the skin with a small surgical blade. Bleeding from the biopsy site is stopped by applying an ointment, a chemical that stops bleeding, or a small electrical current to cauterize the wound.
A shave biopsy is useful in diagnosing many types of skin diseases and in sampling moles when the risk of melanoma is very low. This type of biopsy is not generally used if a melanoma is strongly suspected unless the biopsy blade will go deep enough to get below the suspicious area. Otherwise, if it is a melanoma, the biopsy sample may not be thick enough to measure how deeply the cancer has invaded the skin.
Punch biopsy
For a punch biopsy, the doctor uses a tool that looks like a tiny round cookie cutter to remove a deeper sample of skin. The doctor rotates the punch biopsy tool on the skin until it cuts through all the layers of the skin. The sample is removed and the edges of the biopsy site are often stitched together.
Excisional and incisional biopsies
To examine a tumor that might have grown into deeper layers of the skin, the doctor may use an excisional (or less often, an incisional) biopsy.
- An excisional biopsy removes the entire tumor (along with a small margin of normal skin around it). This is usually the preferred method of biopsy for suspected melanomas if it can be done, although this isn’t always possible.
- An incisional biopsy removes only a portion of the tumor.
For these types of biopsies, a surgical knife is used to cut through the full thickness of skin. A wedge or sliver of skin is removed for examination, and the edges of the cut are usually stitched together.
“Optical” biopsies
Some newer types of biopsies, such as reflectance confocal microscopy (RCM), can be done without needing to remove samples of skin. To learn more, see What’s New in Melanoma Skin Cancer Research?
Biopsies of melanoma that may have spread
Biopsies of areas other than the skin may be needed in some cases. For example, if melanoma has already been diagnosed on the skin, nearby lymph nodes may be biopsied to see if the cancer has spread to them.
Rarely, biopsies may be needed to figure out what type of cancer someone has. For example, some melanomas can spread so quickly that they reach the lymph nodes, lungs, brain, or other areas while the original skin melanoma is still very small. Sometimes these tumors are found with imaging tests (such as CT scans) or other exams even before the melanoma on the skin is discovered. In other cases, they may be found long after a skin melanoma has been removed, so it’s not clear if it’s the same cancer.
In still other cases, melanoma may be found somewhere in the body without ever finding a spot on the skin. This may be because some skin lesions go away on their own (without any treatment) after some of their cells have spread to other parts of the body. Melanoma can also start in internal organs, but this is very rare, and if melanoma has spread widely throughout the body, it may not be possible to tell exactly where it started.
When melanoma has spread to other organs, it can sometimes be confused with a cancer starting in that organ. For example, melanoma that has spread to the lung might be confused with a primary lung cancer (cancer that starts in the lung).
Special lab tests can be done on the biopsy samples that can tell whether it is a melanoma or some other kind of cancer. This is important because different types of cancer are treated differently.
Biopsies of suspicious areas inside the body often are more involved than those used to sample the skin.
Fine needle aspiration (FNA) biopsy
FNA biopsy is not used on suspicious moles. But it may be used, for example, to biopsy large lymph nodes near a melanoma to find out if the melanoma has spread to them.
For this type of biopsy, the doctor uses a syringe with a thin, hollow needle to remove very small pieces of a lymph node or tumor. The needle is smaller than the needle used for a blood test. A local anesthetic is sometimes used to numb the area first. This test rarely causes much discomfort and does not leave a scar.
If the lymph node is just under the skin, the doctor can often feel it well enough to guide the needle into it. For a suspicious lymph node deeper in the body or a tumor in an organ such as the lung or liver, an imaging test such as ultrasound or a CT scan is often used to help guide the needle into place.
FNA biopsies are not as invasive as some other types of biopsies, but they may not always collect enough of a sample to tell if a suspicious area is melanoma. In these cases, a more invasive type of biopsy may be needed.
Surgical (excisional) lymph node biopsy
This procedure can be used to remove an enlarged lymph node through a small incision (cut) in the skin. A local anesthetic (numbing medicine) is generally used if the lymph node is just under the skin, but the person may need to be sedated or even asleep (using general anesthesia) if the lymph node is deeper in the body.
This type of biopsy is often done if a lymph node’s size suggests the melanoma has spread there but an FNA biopsy of the node wasn’t done or didn’t find any melanoma cells.
Sentinel lymph node biopsy
If melanoma has been diagnosed and has any concerning features (such as being at least a certain thickness), a sentinel lymph node biopsy (SLNB) is often done to see if the cancer has spread to nearby lymph nodes, which in turn might affect treatment options. This test can be used to find the lymph nodes that are likely to be the first place the melanoma would go if it has spread. These lymph nodes are called sentinel nodes (they stand sentinel, or watch, over the tumor, so to speak).
To find the sentinel lymph node (or nodes), a doctor injects a small amount of a radioactive substance into the area of the melanoma. After giving the substance time to travel to the lymph node areas near the tumor, a special camera is used to see if it collects in one or more sentinel lymph nodes. Once the radioactive area has been marked, the patient is taken for surgery, and a blue dye is injected in the same place the radioactive substance was injected. A small incision is then made in the marked area, and the lymph nodes are then checked to find which one(s) became radioactive and turned blue. These sentinel nodes are removed and looked at under a microscope.
If there are no melanoma cells in the sentinel nodes, no more lymph node surgery is needed because it is very unlikely the melanoma would have spread beyond this point. If melanoma cells are found in the sentinel node, the remaining lymph nodes in this area are typically removed and looked at as well. This is known as a lymph node dissection (see Surgery for Melanoma Skin Cancer).
If a lymph node near a melanoma is abnormally large, a sentinel node biopsy probably won’t be needed. The enlarged node is simply biopsied.
Lab tests of biopsy samples
Samples from any biopsies will be sent to a lab, where a doctor called a pathologist will look at them under a microscope for melanoma cells. Often, skin samples are sent to a dermatopathologist, a doctor who has special training in looking at skin samples.
If the doctor can’t tell for sure if melanoma cells are in the sample just by looking at it, special lab tests will be done on the cells to try to confirm the diagnosis. These might include:
- Immunohistochemistry (IHC)
- Fluorescence in situ hybridization (FISH)
- Comparative genomic hybridization (CGH)
- Gene expression profiling (GEP)
If melanoma is found in the samples, the pathologist will look at certain important features such as the tumor thickness and mitotic rate (the portion of cells that are actively dividing). These features help determine the stage of the melanoma (see Melanoma Skin Cancer Stages), which in turn can affect treatment options and prognosis (outlook).
Testing for gene changes
For some people with melanoma, biopsy samples may be tested to see if the cells have mutations (changes) in certain genes, such as the BRAF gene. About half of melanomas have BRAF mutations. Some drugs used to treat advanced melanomas are only likely to work if the cells have BRAF mutations (see Targeted Therapy for Melanoma Skin Cancer), so this test is important in helping to determine treatment options. Tests for changes in other genes, such as C-KIT, might be done as well.
A newer lab test known as DecisionDx-Melanoma looks at certain gene expression patterns in melanoma cells to help show if early-stage melanomas are likely to spread. This might be used to help determine treatment options. To learn more, see What’s New in Melanoma Skin Cancer Research?
Imaging tests
Imaging tests use x-rays, magnetic fields, or radioactive substances to create pictures of the inside of the body. They are used mainly to look for the possible spread of melanoma to lymph nodes or other organs. These tests are not needed for most people with very early-stage melanoma, which is very unlikely to have spread.
Imaging tests can also be done to help determine how well treatment is working or to look for possible signs of cancer coming back (recurring) after treatment.
Chest x-ray
This test might be done to help determine if melanoma has spread to the lungs, although a CT scan of the chest (see below) is often done instead.
Ultrasound
Ultrasound uses sound waves to create images of the inside of your body on a computer screen. This test might be used to look at the lymph nodes near the tumor, especially if it’s not clear if they’re enlarged based on a physical exam. Ultrasound is typically fairly quick and easy to do, and it doesn’t expose you to radiation.
Ultrasound-guided needle biopsy: Ultrasound can also be used to help guide a biopsy needle into a suspicious lymph node.
Computed tomography (CT) scan
The CT scan uses x-rays to make detailed, cross-sectional images of your body. Unlike a regular x-ray, CT scans can show the detail in soft tissues (such as internal organs). This test can show if any lymph nodes are enlarged or if organs such as the lungs or liver have suspicious spots, which might be from the spread of melanoma.
CT-guided needle biopsy: CT scans can also be used to help guide a biopsy needle into a suspicious area within the body.
Magnetic resonance imaging (MRI) scan
MRI scans use radio waves and strong magnets instead of x-rays to create detailed images of parts of your body. MRI scans can be very helpful in looking at the brain and spinal cord.
Positron emission tomography (PET) scan
A PET scan can help show if the cancer has spread to lymph nodes or other parts of the body. It is most useful in people with more advanced stages of melanoma.
For this test, you are injected with a slightly radioactive form of sugar, which collects mainly in cancer cells. A special camera is then used to create a picture of areas of radioactivity in the body.
PET/CT scan: Many centers have special machines that do both a PET and CT scan at the same time (PET/CT scan). This lets the doctor compare areas of higher radioactivity on the PET scan with the more detailed appearance of that area on the CT scan.
Blood tests
Blood tests aren’t used to diagnose melanoma, but some tests may be done before or during treatment, especially for more advanced melanomas.
Doctors often test blood for levels of a substance called lactate dehydrogenase (LDH) before treatment. If the melanoma has spread to distant parts of the body, a high LDH level is a sign that the cancer may be harder to treat. This can affect the stage of the cancer (see Melanoma Skin Cancer Stages).
Other tests of blood cell counts and blood chemistry levels may be done in a person who has advanced melanoma to see how well the bone marrow (where new blood cells are made), liver, and kidneys are working before and during treatment.