#patientchat Highlights – Self-Advocacy and Self-Education
Last week we hosted a “Self-Advocacy and Self-Education” Empowered #patientchat on Twitter. Take a look at the top tweets and full transcript from the chat.
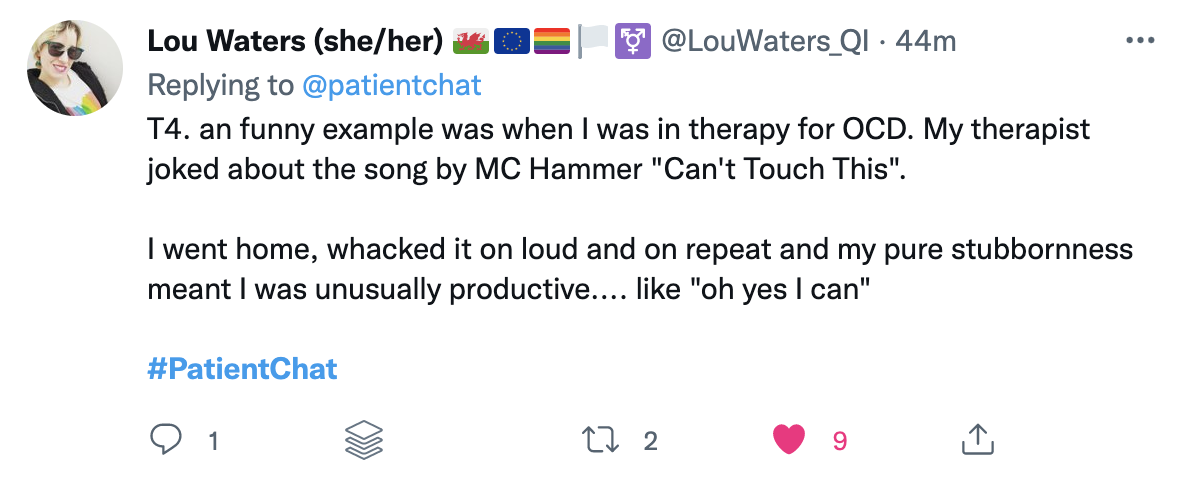
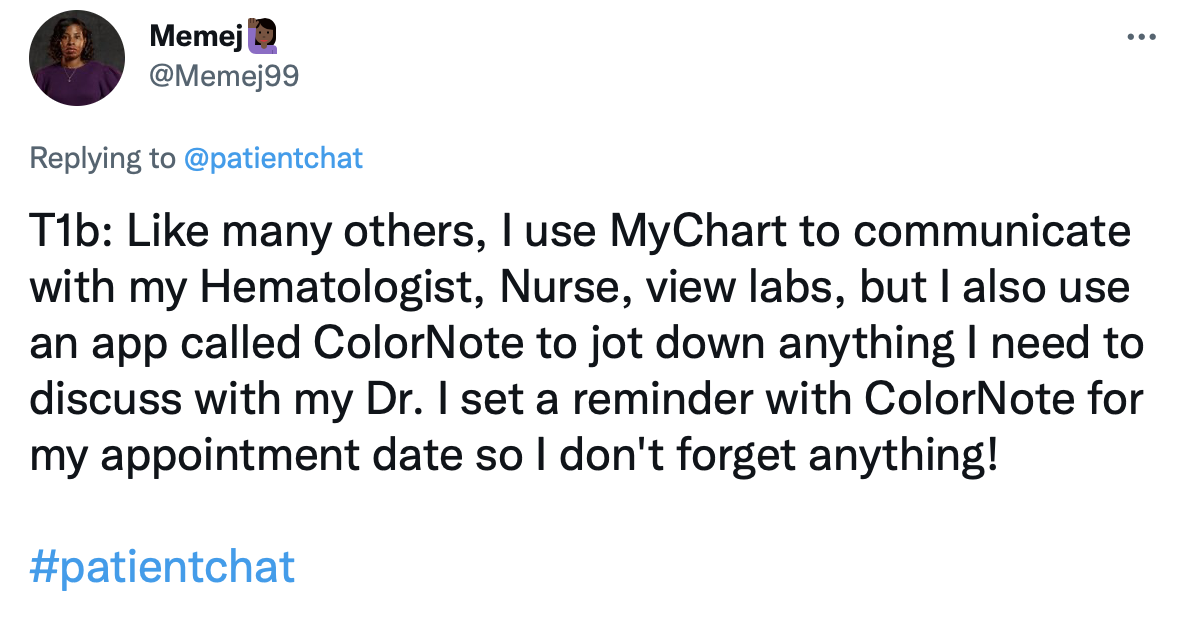
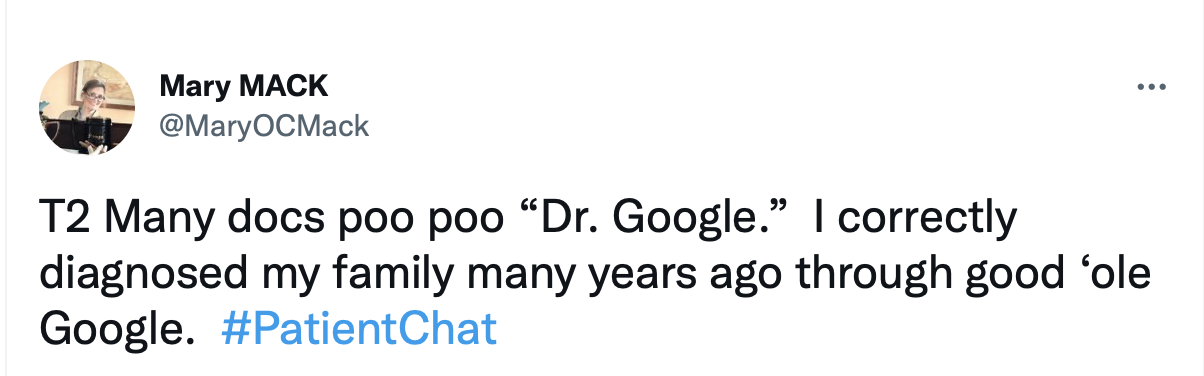
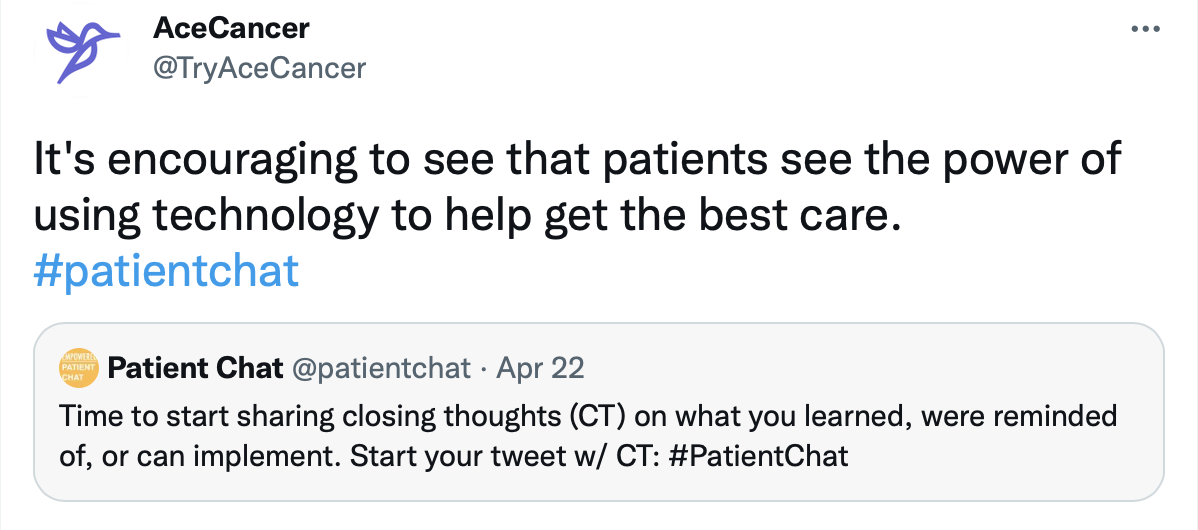
Top Tweets
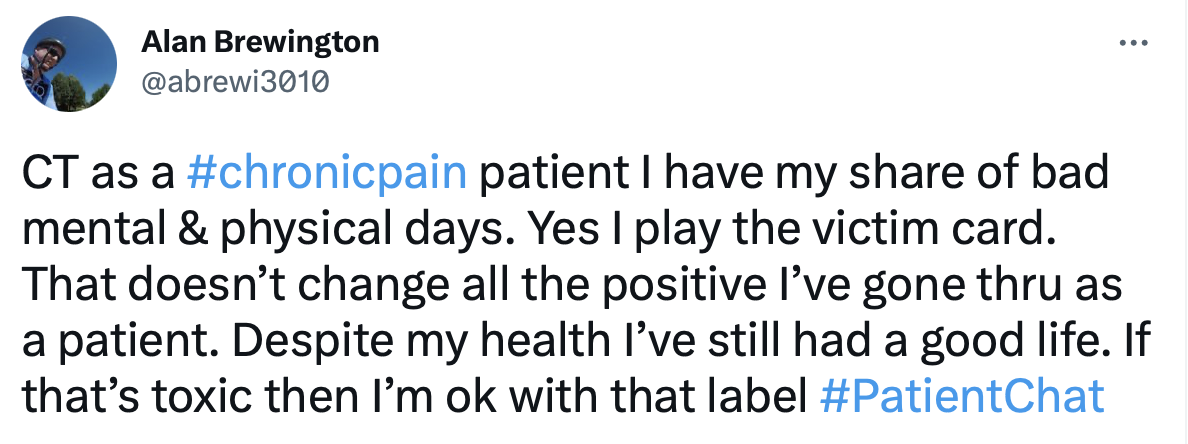
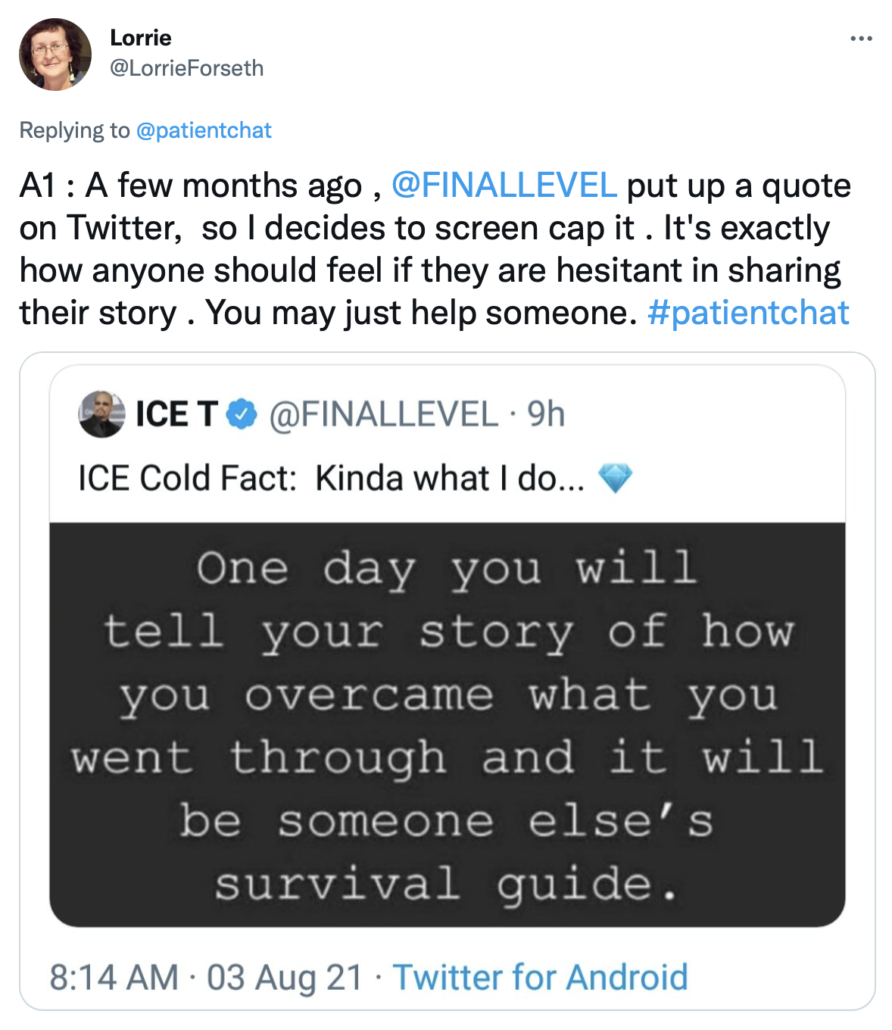
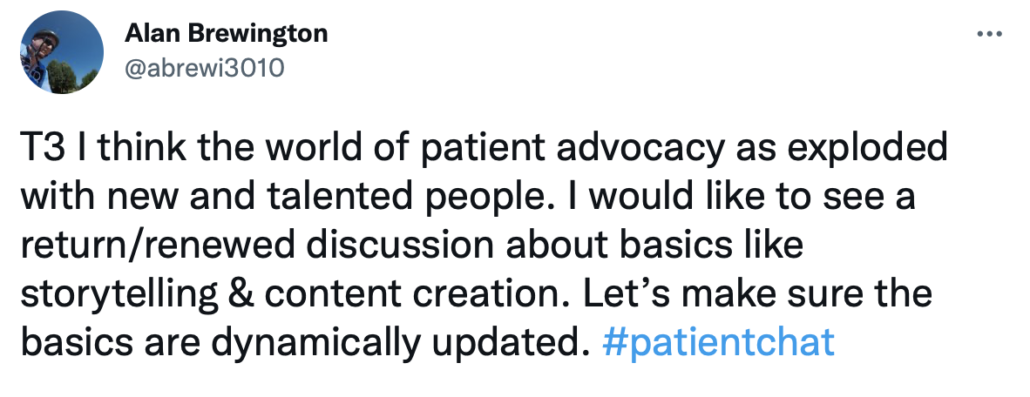
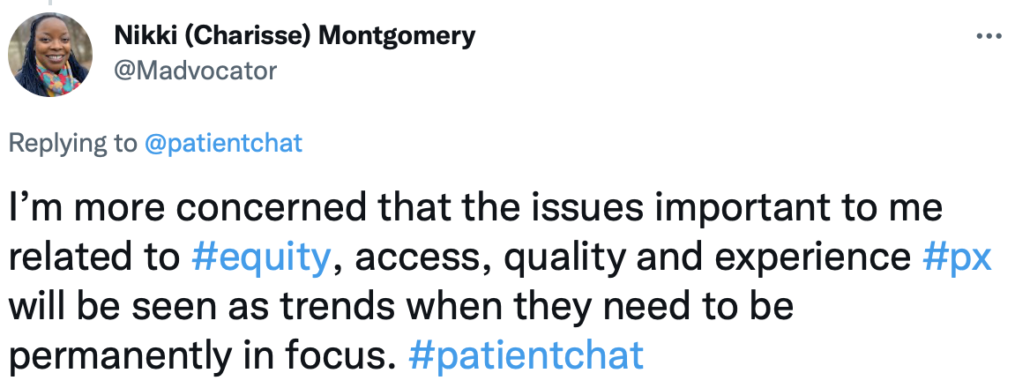
Can you recall a time where advocating for yourself improved your care?
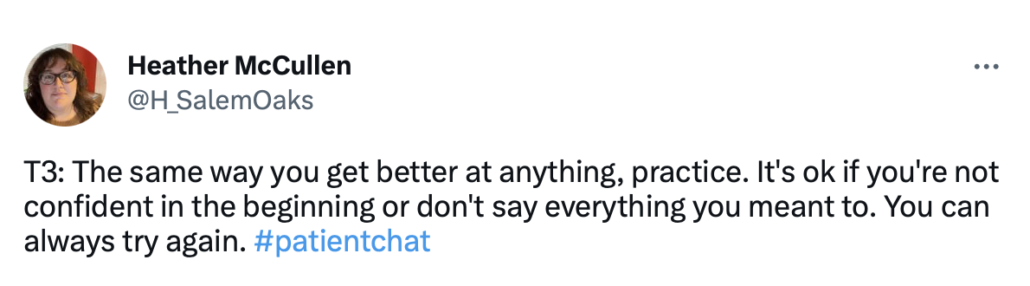
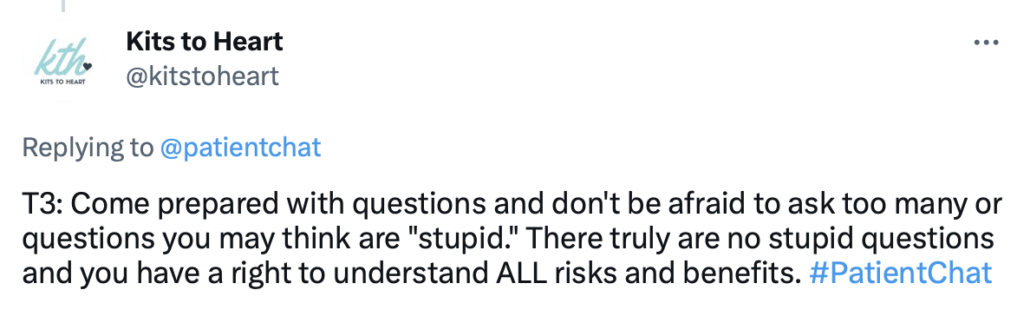
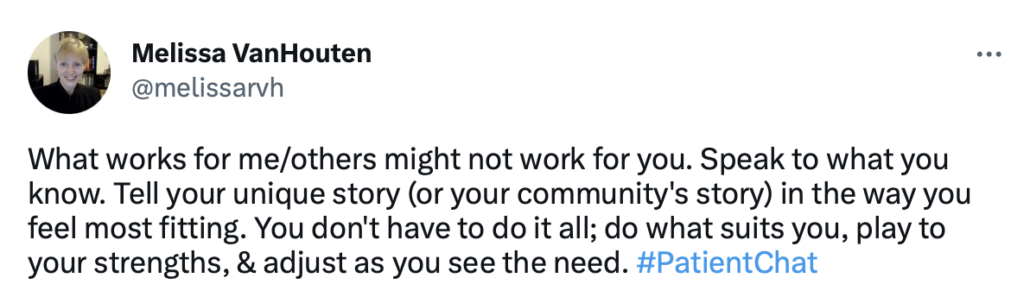
How can you become an effective self-advocate?