Is the COVID Vaccine Effective for CLL Patients?
Is the COVID Vaccine Effective for CLL Patients? from Patient Empowerment Network on Vimeo.
Is the COVID vaccine effective for chronic lymphocytic leukemia (CLL) patients? Dr. Paul Barr shares insight about mRNA-based COVID-19 vaccine effectiveness in CLL patients – both for those in remission and those in active treatment.
Dr. Paul Barr is Professor of Hematology/Oncology at University of Rochester Medical Center. Learn more about Dr. Barr, here.
Related Resources:

|

|

|
Transcript:
Katherine:
I understand that researchers have been looking into whether the COVID vaccination is as effective in people with CLL. What can you tell us about that? The research?
Dr. Barr:
Sure. Everyone knew this was going to be an important question. We’ve known for a long time that riff CLL responses to vaccines in general aren’t as good as some of the normal population. So, there’ve been a whole host of studies over the years where patients didn’t quite respond as well to flu vaccines or pneumonia vaccines. Nonetheless, we typically recommend standard vaccinations, because there’s can be some degree of response. And our testing isn’t always perfect in terms of how well vaccines work.
So, when it typically, is felt to be a relatively safe procedure, is something we typically recommend.
More recently, we looked at studies on the shingles vaccine, and actually that works better than perhaps the flu shot, for example. Because patients probably were previously exposed to that virus earlier in life when they get vaccinated. So, recall response, which is a little bit easier for the immune system.
So, that brings us up to the COVID vaccines, which is obviously critically important ever on everyone’s mind. And the data’s still early. But what we’ve learned so, far is that, like what we might have predicted, our patients, the CLL patients don’t respond as well to the mRNA-based COVID vaccines.
So, in the media we saw, in the larger 20- and 40,000 patients studies that maybe, 95 percent of patients didn’t experience infection. It looks like in the general population, those vaccines work very well. In a cohort of 160, some CLL patients who are vaccinated early on in Israel, it looked like maybe about 40 percent of patients responded.
For the patients who hadn’t previously been treated but had measurable CLL, maybe about half of patients responded adequately in terms of generating antibodies. So, kind of a flip of a coin. For patients who have been treated and were in remission for more than a year, we’ll say the responses were better, maybe 80 percent or so.
For patients who are on active treatment, even our novel treatments, like the BTK inhibitors or venetoclax (Venclexta), the BCL-2 inhibitor, the responses were pretty poor, 18 or so percent.
So, you can see for patients with active disease, their responses are impaired. For those that are in remission, a little better. For those who are on active treatment, the antibody responses aren’t very good. So, I honestly think this is important information, but tell patients, don’t lose hope.
It’s still important to take the precautions. Some degree of wearing masks and social distancing. They will be better protected if their friends and family around them are vaccinated, and they still may respond to some degree. It’s not like the vaccines aren’t working at all. It’s just that the responses aren’t quite as good as the general population. So, again, another long-winded answer, but hopefully that helps patients understand some of the limitations in vaccinations.
But also that generally things are getting safer in that they still can venture out in society, but still have to take some precautions.
What Is a CLL Biomarker?
What Is a CLL Biomarker? from Patient Empowerment Network on Vimeo.
What is a chronic lymphocytic leukemia (CLL) biomarker? Dr. Paul Barr provides the definition of a biomarker and explains how they may assist in determining a CLL patient’s prognosis and treatment approach.
Dr. Paul Barr is Professor of Hematology/Oncology at University of Rochester Medical Center. Learn more about Dr. Barr, here.
Related Resources:

|

|
Transcript:
Katherine:
Often patients are confused with the term biomarker or biomarker testing. Would you define that for us?
Dr. Barr:
Sure. Biomarkers, I think of them as surrogates to understand the bigger picture. A lot of times what we really want to know when we’re meeting a patient is what’s going to happen in the future? What’s going to happen in five and 10 years from now? Or maybe we want to know as we’re getting closer to treatment, how well is this going to work and how long is it going to work for?
So, we do a lot of research in developing surrogate tests to try to give us an idea of what the future might hold. And so, we have developed a number of molecular genetic tests that we test for, and they give us an estimate of what to expect in terms of the patient’s prognosis.
Or perhaps they help predict for which treatment might work best. So, we often, will look at some molecular aberrations or some genetic tests that tell us about abnormalities just within the CLL cells in the leukemia cell. And they can predict for more slowly or rapidly growing disease. And other tests, might predict for, which drug might serve a patient best in terms of efficacy or how long would it work or for safety.
So, think of that as useful tools to help us give the patients an idea of what to expect over time.
An Expert’s Perspective on CLL Research Advances
An Expert’s Perspective on CLL Research Advances from Patient Empowerment Network on Vimeo.
What chronic lymphocytic leukemia (CLL) research advances have emerged recently? Dr. Paul Barr shares how CLL treatments have advanced in recent years and how progress has impacted quality of life for patients.
Dr. Paul Barr is Professor of Hematology/Oncology at University of Rochester Medical Center. Learn more about Dr. Barr, here.
Related Resources:

|

|
Transcript:
Katherine:
What are you excited about when it comes to CLL research?
Dr. Barr:
Well, it’s hard not to be excited, honestly. Five years ago, roughly, we were largely using chemotherapy.
And while patients could do very well, not all of them did. And in such a short period of time, everything has been turned on its head. We have better treatments for safer, patients are doing better, they’re living longer. There are more novel treatments being studied now. And we start to wonder if with some of the newer treatments, if maybe we actually can cure this disease. Maybe if the majority of them, they might be able to live a normal lifespan. So, we’re incredibly optimistic.
Those are very general statements, but they really are, they come from just the impressive outcomes that we’ve seen from patients being able to be at home, take their treatment, go into deeper remissions and do better in the long-term.
So, yeah, there’s a lot to be excited about. And that’s why my answer is just kind of general. There’s a lot to focus on, from the different novel agents to MRD-guided therapy, to some of the CAR-T products that are coming out. I really think it’ll continue to change at a pretty rapid pace.
Katherine:
That sounds very promising. When it comes to new developments in research, how can patients discuss this type of information with their doctor to find out if there’s a new approach or a clinical trial that might be right for them?
Dr. Barr:
Well, I honestly think they should feel empowered to simply ask. I know a lot of my patients they will want to know anything new. They can ask us, generally is that, they know that we have these major meetings twice a year. And what’s new with these treatments. Or many of them are on clinical trials and want to know, “Do we have any results yet? What’s been changing?” And sometimes at the end of every visit, we’ll spend five minutes just talking about the new developments or what’s coming down the pike or how practice is changing.
I’m just in the routine of having this conversation with most of the patients on a recurring basis. And honestly, they feel well-served, like we’re keeping them up to date. I think patients enjoy that sort of conversation. So, I wouldn’t feel shy about simply asking.
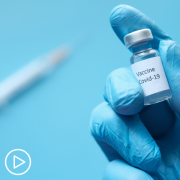
How Can You Engage in Your CLL Care?
How Can You Engage in Your CLL Care? from Patient Empowerment Network on Vimeo.
How can chronic lymphocytic leukemia (CLL) patients become more engaged in their care? Dr. Paul Barr explains steps that patients can take to activate shared decision-making with their provider for optimal care.
Dr. Paul Barr is Professor of Hematology/Oncology at University of Rochester Medical Center. Learn more about Dr. Barr, here.
Related Resources:
|

|
Transcript:
Katherine:
We’ve been hearing a lot about shared decision-making lately. In your opinion, how is this concept best put into practice?
Dr. Barr:
So, I honestly think shared decision-making is not just useless term. This is something we actually really use in our clinics, and it’s very important for the care of CLL patients, where we have patients who do very well for a long period of time. And there are a lot of different management decisions and a variety of treatment options that we have to discuss.
So, when we have that luxury, it’s really important to help educate patients on the different options and to better understand what their goals of care are, so they can help us decide what’s best for them. When we’re deciding just, one example is that, when we’re deciding on various treatments, we can use agents that are given orally, taken at home, but patients may be on them for many years.
Alternatively, we have fixed duration regimens, but may involve trips to the infusion center. And a lot of these different treatments all work very well. So, involving the patient in that decision making process, makes the process that much easier for the patient and enables you just to take better care of them over the long run.
Katherine:
What is the role of the patient to making treatment decisions?
Dr. Barr:
Well, I think that the role of the patient is really to be their own advocate. Take all the information and then, help us make decisions together. And to just be very honest about what they want from, not just a simple decision about a treatment, but from their overall care. To really just to be as involved as possible and to make sure all of their concerns are heard, all of their questions are answered.
Katherine:
For those who might have trouble speaking up for themselves, what advice do you have for them?
Dr. Barr:
Oh, I would say, especially for our patients with CLL, often there are many,
many appointments along the way, where there may not be urgent decisions being made and there are opportunities to slowly learn more to ask questions. So, as much as possible, try not to be intimidated by that visit to the cancer center, which obviously can be anxiety provoking, but to develop a relationship with your hematologist, your oncologist, your care team so, that they can take better care of you.
I honestly think it works best when you slowly get to know your team, understand the field, some of the decisions that need to be made and that the team only wants what’s best for you. So, yeah, I honestly think it’s – think of it as a process. It’s not a one-time visit where you have to get everything out and get everything answered. It should be a relationship.
CLL Treatment and Research Update: News from ASCO 2021
CLL Treatment and Research Update: News from ASCO 2021 from Patient Empowerment Network on Vimeo.
What’s the latest chronic lymphocytic leukemia (CLL) treatment and research news out of the American Society of Clinical Oncology (ASCO) 2021 meeting? Dr. Paul Barr shares study results and explains how they could impact CLL care.
Dr. Paul Barr is Professor of Hematology/Oncology at University of Rochester Medical Center. Learn more about Dr. Barr, here.
Related Resources:

|

|
Transcript:
Katherine:
I’m Katherine Banwell, your host for today’s program. Joining me is Dr. Paul Barr. Dr. Barr, would you please introduce yourself?
Dr. Barr:
Sure. Hi, Paul Barr from the University of Rochester. Glad to be here.
Katherine:
Thank you so, much. Cancer researchers came together recently to share findings at the annual American Society of Clinical Oncology meeting, also known as ASCO. Is there news from the meeting that CLL patients should know about?
Dr. Barr:
There is. It seems like at every major meeting, we have a potentially practice-changing dataset that we like to scrutinize and talk about. This ASCO is no exception. I think probably the most impactful abstract was a report.
The first time we’ve seen the results from a study that was called The ELEVATE Relapsed Refractory Study. This was a randomized trial, enrolling previously treated CLL patients who had high-risk disease and randomizing them to two of our very important BTK inhibitor treatments.
Half the patients got acalabrutinib (Calquence), and the other half received ibrutinib (Imbruvica). And both groups were treated until the drug essentially either stopped working, the disease became resistant or was stopped for side effects. So, this was a study we have waited on the results for a long time given that we don’t often see these randomized studies comparing two such active agents. And the results showed us that both drugs work really almost equally as well.
The progression-free survival or the roughly the average amount of time patients are taking the drug was just over three years, 38 months in both arms. So, they really work very well and equally as well. But we did see less side effects with the acalabrutinib. And one of the most important side effects that the study was powered around was, atrial fibrillation or flutter.
There was less AFib or less new AFib in patients that were treated with the acalabrutinib. There was also less minor bleeding, arthralgia, diarrhea. So, a number of, perhaps less severe type side effects, were less common. There was more headache and more cough in the acalabrutinib-treated patients. But I think overall, most of us took from this abstract that both drugs work exceptionally well.
And overall, are very well tolerated treatments although there does look to be lower rates of a number of important side effects with acalabrutinib.
Katherine:
Dr. Barr, is there any other news from the conference that patients should know about?
Dr. Barr:
There is. I’ll give you a couple other additional findings. One was an update of a study, we’ve seen the results before. It’s sort of a partner study to the one I just mentioned. It was called The ELEVATE TN or ELEVATE Treatment Naive Study.
These were previously untreated patients, treated with an old standard, randomized study where the patients received either chlorambucil-based therapy (Leukeran). It was combined with a CD20 antibody obinutuzumab (Gazyva). The second arm was single agent acalabrutinib and the third arm was acalabrutinib plus obinutuzumab. Not surprisingly both of the acalabrutinibs continue to perform very well. The treatments work much better than chlorambucil. But now, we have four-year data. And that’s important for us to really understand what to expect as time goes on.
And I think that the major take-homes are that, acalabrutinib continues to work very well in the first-line setting. There is a hint that acalabrutinib, I’m sorry, that obinutuzumub may prolong the remissions, which is a little bit surprising to us.
But again, small differences in the study weren’t powered to really look at that comparison. And also, the major take home from that dataset is that the safety still looks very good at four years for the patients receiving acalabrutinib. So, I think that continues to shape our practice. And I think the last dataset or abstract to comment on, was one actually we saw at a different meeting at the European Hematology Association meeting, EHA. And this was another randomized study comparing two different BTK inhibitors in relapsed CLL patients.
This one compared ibrutinib and zanubrutinib (Brukinsa). Like acalabrutinib, zanubrutinib is another more specific BTK inhibitor. And when you compare it to ibrutinib and perhaps somewhat similarly to The ELEVATE Relapsed Refractory Study in this zanubrutinib-ibrutinib comparison, so-called ALPINE study, we saw similar efficacy.
Zanubrutinib actually looked like it performed a little better than ibrutinib, but also again here, lower rates of side effects. So, the theme continues for the more specific BTK inhibitors. They seem to work just as well, maybe a little better in some respects, compared to Ibrutinib and somewhat lower rates of side effects. So, when you put it all together, all of the BTK inhibitors work exceptionally well.
We have varying degrees of follow-up and confidence. We have the most follow-up in our ibrutinib treated patients so, we know what to expect for patients six, seven years out after being on ibrutinib.
But we’re now seeing in these earlier studies that lower rates of various toxicities for the newer more specific BTK inhibitors. So, kind of a long-winded answer to your simple question, but hopefully that shows how the new and emerging data continues to shape how we take care of patients.
NCCN Guidance on Safety and Effectiveness of COVID-19 Vaccines for Cancer Patients
NCCN Guidance on Safety and Effectiveness of COVID-19 Vaccines for Cancer Patients from Patient Empowerment Network on Vimeo.
Is the COVID-19 vaccine recommended for people living with cancer? Dr. Erin Roesch shares recommendations from the National Comprehensive Cancer Network (NCCN) for those undergoing cancer treatment, including guidance on mask wearing and advice for family members.
Dr. Erin Roesch is a breast medical oncologist at the Cleveland Clinic. Learn more about Dr. Roesch here.
Transcript:
Katherine:
Many cancer patients have questions about the COVID vaccine. Is it safe? Do we need to continue wearing masks? Here to address these questions is cancer expert, Dr. Erin Roesch. Dr. Roesch, would you introduce yourself?
Dr. Roesch:
Hello. And thank you for inviting me to participate in this very important conversation. My name is Erin Roesch. I am a breast medical oncologist at Cleveland Clinic.
Katherine:
Excellent. Thank you so much for joining us today. I’d like to run through a list of concerns that cancer patients have about vaccines in general and the COVID vaccine specifically.
So, let’s start with a basic question. Should people get vaccinated if they have cancer?
Dr. Roesch:
Yes. All individuals diagnosed with cancer should get the COVID-19 vaccine as recommended by the National Comprehensive Cancer Network or NCCN.
An immunocompromised state makes many people with cancer at higher risk of serious COVID-19 illness. Those who are vaccinated are less likely to become sick with COVID-19. And, also, vaccinated people who do get COVID-19 are much less likely to become seriously ill.
I would also mention that those living in the same household as a person diagnosed with cancer and caregivers or other close contacts should also get vaccinated.
Katherine:
Another common question is whether people with cancer should wait for any reason to get the COVID-19 vaccine.
Dr. Roesch:
Most people with cancer should get the vaccine as soon as they can with a few exceptions according to NCCN.
People in the process of receiving stem cell transplant or cellular therapy should wait at least three months after they finish treatment to get vaccinated.
Those diagnosed with certain forms of leukemia should also wait a few weeks after receiving treatment to allow their immune system to recover so the vaccine can be effective.
It’s not been clearly defined exactly how chemotherapy affects responses to COVID-19 vaccines. But some data suggests that immune responses may not be as robust. However, it is still recommended that those receiving chemotherapy and also immunotherapy and radiation should get vaccinated whenever they can.
Katherine:
I think a lot of people are concerned too about whether one vaccine is better than another. What would you say to them?
Dr. Roesch:
And that is a common question that I often get in my clinic. And I advise my patients to receive or take whatever vaccine they are offered.
We don’t really have any studies or data at this point suggesting one being better than another in cancer patients.
Katherine:
Some people are wondering if the vaccine can give a person COVID-19. How would you address that?
Dr. Roesch:
I would say that as none of the currently available vaccines are made with a live virus, the vaccine itself can’t give a person COVID-19. By getting vaccinated, actually, those who are immunocompromised are really helping society to prevent the spread of COVID-19. Immunocompromised people who get COVID-19 may be more likely to infect others due to prolonged shedding of the virus after infection.
Katherine:
What about side effects? Are the vaccine’s side effects worse for people with cancer?
Dr. Roesch:
No. Side effects do not appear to be worse for those diagnosed with cancer. Results to date suggest that the vaccine’s side effects in people with and without cancer are really no different.
These side effects, as we have seen, may include arm soreness, rash, fatigue, chills, fever, headache, for example.
Katherine:
And, finally, can cancer patients stop wearing a mask after they’ve been vaccinated?
Dr. Roesch:
Cancer patients should continue to wear a mask post-vaccination. Many people with cancer may have a harder time actually fighting infections and may not respond as well to vaccines. So, people diagnosed with cancer and their close contacts should get vaccinated and then continue to follow precautions, which include wearing masks, social distancing, hand hygiene.
Katherine:
Is there a certain length of time that people need to continue wearing a mask after being vaccinated?
Dr. Roesch:
At this time, I would recommend patients continue to follow the CDC guidelines that are currently in place. And at this point, I don’t think we have a projected end time for that yet.
Katherine:
Is there anything else you’d like to share with cancer patients who may be concerned about vaccinations?
Dr. Roesch:
I would encourage those diagnosed with cancer to not only themselves get vaccinated but to also really voice and stress the importance of vaccination to those that surround them, including, again, members of their household, close contacts, and even beyond their inner circle.
I would also advise people to try and avoid letting the concern of possible side effects related to the shot deter them from getting it. The symptoms of COVID-19 can be much worse and potentially serious for some compared with the relatively minor side effects that we’ve seen with the vaccine itself.
I also would mention I’ve had personal patients that have expressed concern about functioning of their immune system while receiving chemotherapy and how this might affect their response to the vaccine. I do emphasize to them that even though responses might not be as strong as they may be in the absence of active treatment, I feel like the potential benefits of the vaccine still outweigh the risks in my mind.
Katherine:
Thanks so much for joining us today, Dr. Roesch.
Dr. Roesch:
Thank you for having me.
How to Make Confident and Informed CLL Treatment Decisions
How to Make Confident and Informed CLL Treatment Decisions from Patient Empowerment Network on Vimeo.
How can you engage effectively in your CLL care? Collaborating with your doctor and playing an active role in your care can lead to improved outcomes. This animated video reviews essential steps and important considerations for making informed and confident CLL treatment decisions.
Related Resources:

|

|

|
Transcript:
Elena:
Hi, I’m Elena and this is my husband, Bill.
Elena:
Several years ago, I was diagnosed with CLL, which stands for chronic lymphocytic leukemia. CLL is a blood cancer that starts in the bone marrow. It’s the most common type of adult leukemia.
When I was first diagnosed, I wasn’t treated right away. It was confusing at the time, but my CLL doctor, Dr. Singh, told me that most people with CLL don’t need to be treated immediately.
Here’s Dr. Singh, he can explain it further.
Dr. Singh:
Hi! I’m Dr. Singh, and I’m a hematologist specializing in the care and treatment of people with CLL.
At first, we approached Elena’s CLL with “watch and wait” or active surveillance. Through physical exams, blood work and frequent communication, we monitored how her CLL was progressing over time.
Elena:
I was in watch and wait for about a year—then, I begin to have symptoms that interfered with my daily life. I had drenching night sweats and I felt so exhausted.
Dr. Singh:
Right! An increase in symptoms is often an indicator that it’s time to treat a patient’s CLL. Elena’s fatigue and night sweats are common symptoms. Other symptoms can include enlarged lymph nodes or spleen, fever, unintentional weight loss and frequent infections.
In addition to an increase in symptoms, signs that it might be time to treat can include anemia or low platelet counts.
Elena:
So, once Dr. Singh let me know it was time to treat my CLL, he walked me and Bill through the goals of treatment.
And by that, I mean we discussed balancing my lifestyle with finding an effective treatment for my CLL.
Dr. Singh:
Elena let me know that she’s very social and enjoys riding her bike – we wanted to make sure she could continue doing the activities she loves.
The clinical goals of CLL treatment are to slow, stop or eradicate the cancer. I spoke with Elena and Bill about finding an approach that may get her CLL under control while preserving her quality of life.
Elena also had essential testing, including biomarker testing, which we took into consideration along with her treatment goals. We reviewed each potential approach to make sure we found the best, most personalized treatment option for HER CLL.
We discussed the effectiveness of the treatment option, and the likelihood of a recurrence a. And we reviewed what our next steps would be if the treatment plan needed to be adjusted.
Bill:
And I wanted to make sure Elena was able to continue feeling her best, so I asked about potential side effects for each therapy and how it could impact our lifestyle.
Dr. Singh:
Exactly! We discussed how each treatment option could affect Bill and Elena’s daily life. You and your doctor may also consider:
- The financial impact of a treatment plan
- Your age and overall health
- The stage of your disease at the time of treatment
- And Biomarker test results
Elena:
In addition to asking questions, Bill took notes during our appointments, since it was often hard for me to absorb everything at once.
Bill:
We also made sure to talk about the appointment on our way home, while the information was fresh on our minds. And we did our part by researching CLL and bringing a list of questions to each appointment.
I found an office visit planner on the Patient Empowerment Network website that helped me organize my health info and questions.
Dr. Singh:
As you can see, Bill and Elena were actively engaged in each care decision. It’s vital that patients feel empowered to speak up. If you can, bring a friend or loved one along to your appointment.
And, if you are able, it’s a good idea to seek a second opinion or a consultation with a CLL specialist to help you feel confident in your care decisions.
Elena:
Dr. Singh made Bill and I feel included in the decision-making process, as if it were a collaboration.
Dr. Singh:
That’s right. This is a partnership. So, what steps can you take to be more engaged in your CLL care?
- Understand and articulate the goals of your CLL treatment plan.
- Learn about your options and weigh the pros and cons of each approach.
- Bring a friend or loved one to your appointments.
- Ask about essential testing and how it may impact your treatment options.
- Consider a second opinion or a consult with a CLL specialist.
Bill:
That’s great advice, Dr. Singh. To learn more, visit powerfulpatients.org/CLL to access a library of tools.
Elena:
Thanks for joining us.
How Can CLL Patients Be Active in Their Care Decisions?
How Can CLL Patients Be Active in Their Care Decisions? from Patient Empowerment Network on Vimeo.
How can chronic lymphocytic leukemia (CLL) patients take a more active role in their care decisions? Dr. Matthew Davids details considerations for CLL treatment and explains ways that patients can take action to ensure their patient voice is heard for their care.
Dr. Matthew Davids is Director of Clinical Research in the Division of Lymphoma at Dana-Farber Cancer Institute. Learn more about Dr. Davids here.
Related Resources:

|

|
Transcript:
Katherine:
Lately we’ve been hearing the term “shared decision-making,” which basically means that patients and clinicians collaborate to make healthcare decisions.
And it can help patients take a more active role in their care. What are your thoughts, Dr. Davids, on how best to make this process work?
Dr. Davids:
Yeah, I fully support that model. I think for most patients it’s very helpful to be an important decision-maker. Really the patient is the ultimate decision-maker to say what they want for their own treatment. And sometimes it’s hard for me to predict what a patient will want for themselves, so I see my role for most patients as providing the information that they need to make the best decision possible for themselves.
I do try to steer patients a bit in the directions that I think they should be thinking. I’m not going to necessarily present a laundry list of things to patients. I’m going to try to narrow it down to what I think are the most reasonable choices for a patient to make.
I feel that’s part of my job. I do still have patients who just say, “Just tell me what to do,” and I respect that, too. Not all patients want to be part of shared decision making, and they just want me to decide, and that’s fine. But I do find that most patients like the idea of having a voice and being the one to decide, and that way I can help to guide them, but ultimately, it’s up to them.
Katherine:
Well, speaking of patients having a voice, are there questions that patients should consider asking when they’re thinking about a proposed treatment plan?
Dr. Davids:
Yeah. I think some of the key ones revolve around basic stuff, but sometimes it’s hard to think of it in the moment. But thinking about, what are the risks of this therapy? What are the specific side effects that are most common? When you look at a package insert or you look at a clinical trial consent form, you’re going to see 100 different side effects listed. I always promise patients, “You won’t have every single side effect that’s listed here, but you may have a couple of them.” And again, my role often is to identify which are the more common side effects that we see and how can those be managed?
And then, I think often you’re just asking simply about what are the potential benefits of this therapy? What are the odds that I’m going to get into remission? How long is this remission likely to last?
And then, something that is often challenging for patients to think about – it can be challenging for me as well – is to think about what’s the next step? So, I think a good question to ask is, “If I choose Therapy A, what happens if I need therapy again in a few years? What are the options at that point?” because we’ve been talking so far mostly about what we call frontline therapy, making that initial choice of treatment. But then, once you get into what we call the relapse setting, a lot of the decision of what to receive at that point depends on what you got as the first therapy. And so, trying to think at least one step ahead as to what the next options are I think can be helpful, certainly for the physicians but also for the patients.
Katherine:
Do you have any advice to help patients speak up when they’re feeling like their voice isn’t being heard?
Dr. Davids:
That’s always a challenging situation, but I encourage patients not to be shy about asking questions.
There’s often an imbalance in terms of the information where the oncologist may know more than the patient about a particular condition. And so, I think reading up and trying to educate yourself as much as you can. Whenever possible, including a family member or friend as part of the visit to also help advocate for you. And then, if you’re not being heard the way that you think you should be, thinking about seeking out another provider who may be able to listen more.
And sometimes that can be again helpful to have a touchpoint with a CLL specialist who may be able to reinforce some of what you’re thinking. If what you’re reading online or seeing online is different from what your oncologist is telling you, that may be a sign that it’s good to get a second opinion and just make sure you’re on the right track.
What Are the Goals of CLL Treatment?
What Are the Goals of CLL Treatment? from Patient Empowerment Network on Vimeo.
What are some of the goals of chronic lymphocytic leukemia (CLL) treatment? Dr. Matthew Davids outlines some different treatment goals and how the goals are impacted by a patient’s age and other considerations.
Dr. Matthew Davids is Director of Clinical Research in the Division of Lymphoma at Dana-Farber Cancer Institute. Learn more about Dr. Davids here.
Related Resources:

|
Transcript:
Katherine:
With CLL, what are the goals of treatment?
Dr. Davids:
I like to say to patients, “The goals are to make you live longer and live better.” You want to obviously have treatments that prolong life, but you also want to have treatments that are helping with symptoms, and giving patients more energy, and making them feel better, and protecting them from some of the risks of the disease. And so, I think the goals do vary a bit based on the stage of life that patients are at.
I see a lot of patients in their 70s and 80s, and in those patient’s symptom control, having the disease be in a good remission, allowing them to live their life is a good goal. I sometimes see patients in their 40s and 50s, and some of those patients want to be a bit more aggressive and try to do a strategy that will get them a very long-term remission, and even potentially explore potentially curative strategies.
If I have a higher-risk patient with deletion 17p who’s young and fit, and they’ve already had some of the novel treatments, that’s where we start thinking about clinical trials of some of the cellular therapies like CAR-T cells that people may have heard of where you use the T cells from the patient to try to use that as a therapy to kill off the disease. Or even a bone marrow transplant is something that we have used historically in CLL. We don’t use it as often now, but for younger patients with high-risk disease it’s still a consideration to try to achieve a cure of the CLL even though the risks of that are significant.
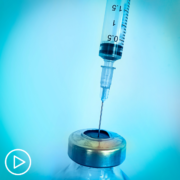
What Should CLL Patients Know About Clinical Trial Treatment Options?
What Should CLL Patients Know About Clinical Trial Treatment Options? from Patient Empowerment Network on Vimeo.
What do chronic lymphocytic leukemia (CLL) patients need to know about clinical trial treatment options? Dr. Matthew Davids explains how clinical trials fit into the array of CLL treatments, the benefits of speaking to a CLL specialist, and online resources for finding clinical trials.
Dr. Matthew Davids is Director of Clinical Research in the Division of Lymphoma at Dana-Farber Cancer Institute. Learn more about Dr. Davids here.
Related Resources:
|

|
Transcript:
Katherine:
Right. Where do clinical trials fit in with the treatment approaches?
Dr. Davids:
So, clinical trials are really how we’ve made all these advances in CLL over the last decade. It’s how we learn about new treatments. It’s how we learn about how to optimize the treatments that we have. I think sometimes patients have a misconception that clinical trials are a last resort, the idea that you’ve exhausted all the standard options and then you go to a clinical trial as your last hope. But I actually like to kind of turn that on its head and say that clinical trials are actually the first resort, the first best option for patients. Whenever patients can get access to a clinical trial at any stage of their disease, I would really encourage them to consider it.
We have quite a few clinical trials now in the frontline setting, meaning as an initial treatment for CLL, including some that are in development and will open soon. And these are the studies that are going to really help us define what the optimal regimens are. What’s the optimal sequence of these different novel agents?
And in CLL, really, we’re at a point where the research on the disease is so mature that when you’re in a clinical trial you’re either going to be on one regimen that you know you’re getting and you know it’s going to be an effective regimen, or you might be in a comparative trial where you could be randomized to one of two or three different regimens, but you know that each one of those regimens is one that we think is a great regimen. We just don’t know which one is optimal for individual patients. So, this is not a situation where there’s placebo-controlled trials where you don’t know if you’re going to get an active treatment or not. CLL is an area where we design our clinical trials so that all patients are going to be benefiting from cutting-edge approaches.
And so, not all patients have access to trials, and that’s okay. Again, we’re fortunate that we have many good options that can be given locally, but I do encourage patients even if they’re only able to travel to a CLL specialist once to have an initial consultation to think about doing that to get a CLL specialist on your team, so to speak. That way they can identify clinical trial options that may be a good fit, and even if not, they can advise on what the optimal treatment options are to receive locally with your own oncologist.
Katherine:
How do patients find out about these clinical trials?
Dr. Davids:
I do think the best way is through a CLL specialist because certainly they would have a great pulse on the trials, they have available at their own center. They should also have a sense for what trials are available maybe at other centers. Some of that can also be, there’s a great resource through The Leukemia & Lymphoma Society where they can help navigate patients toward specific trials that may be applicable to them.
There’s also a website called clinicaltrials.gov. It can be a little challenging if you’re not familiar with it to navigate the site, but it is actually pretty straightforward. You can put in the disease and look at different options for trials based on different drugs, for example. They’ll list the eligibility criteria for the trial. That’s often I find a way that patients can begin to identify whether they may be a candidate. You can’t tell from the website whether you’re definitely a candidate or not. You really need to partner with an investigator who’s on the trial to learn that, but it certainly can be a good starting point to figure out what’s out there.
An Overview of CLL Treatment Types
An Overview of CLL Treatment Types from Patient Empowerment Network on Vimeo.
What are the treatment types for chronic lymphocytic leukemia (CLL)? Dr. Matthew Davids details each type of treatment – and which type of patients some treatments may be most appropriate for.
Dr. Matthew Davids is Director of Clinical Research in the Division of Lymphoma at Dana-Farber Cancer Institute. Learn more about Dr. Davids here.
Related Resources:

|

|
Transcript:
Katherine:
Well, once it’s time to treat, of course, then it’s time to think about treatment options. Let’s walk through the types of treatments that are used today to treat CLL.
Dr. Davids:
As I alluded to before, we historically have had chemotherapy-based approaches to treat CLL. And that was an effective way to temporarily put the disease into remission, but it had a lot of side effects and inevitably the CLL would come back. And the challenge particularly with chemotherapy-based approaches it that when the CLL does come back after chemotherapy, it tends to behave more aggressively and be harder to treat.
So, there have been quite a few studies over the last few years trying to figure out ways that we can avoid using chemotherapy as the first treatment, and this can involve treatments such as monoclonal antibodies. People may have heard of rituximab or a newer drug, obinutuzumab. There are the inhibitors of the B-cell receptor pathway, and this is for example ibrutinib (Imbruvica), which targets a protein called BTK, also a newer one called acalabrutinib (Calquence), which targets BTK. And then, I mentioned at the beginning these fixed-duration therapies that stop after a period of time. Many of those are based on a newer oral drug called venetoclax (Venclexta), which when we give it as a first therapy, we give in combination with that antibody obinutuzumab (Gazyva).
So, a bit of an alphabet soup. I know it gets confusing with all the different treatments, but the good news for CLL patients is, 1.) we have a lot of options, which is great, 2.) we don’t necessarily need to use chemotherapy anymore, and in fact I use it pretty rarely these days. One situation where I do still consider chemotherapy is for younger patients – which in the CLL world is sort of under age 60 or so – if they have very favorable biology to the disease, in particular this mutated IGHV.
That’s a scenario where the older chemotherapy regimen, FCR, can be very effective. It’s a six-month treatment, and we have patients with those molecular characteristics who are now 12, almost 15 years out from their initial six months, and they’re still in a complete remission. So, many of those patients have been functionally cured of their CLL from the six months of treatment. But again, there are some risks to that approach. We worry about other cancers that may be more likely after receiving FCR. We worry about infections, and particularly in the COVID situation, we worry about COVID infection in patients on chemotherapy.
So, it’s been pretty rare that I’ve been using that approach these days. I’ve been opting more for the novel agent-based approaches. So, often now the conversation as an initial therapy comes down to, “Do you prefer more of a continuous treatment strategy with a BTK inhibitor drug like ibrutinib or acalabrutinib, or do you like the idea of a time-limited therapy with one year of venetoclax in combination with obinutuzumab?” And I would say there’s pros and cons to both approaches, and we don’t know which one is the optimal one for CLL patients to start with, but probably I think most patients at some point in their lifetime are going to need one therapy or the other.
So, maybe in the end it doesn’t matter too much which one you start with if you’re going to get both eventually anyway. But we don’t know that yet.
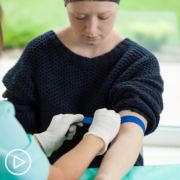
How Does CLL Progress? Understanding the Stages of CLL
How Does CLL Progress? Understanding the Stages of CLL from Patient Empowerment Network on Vimeo.
What are the specific stages of chronic lymphocytic leukemia (CLL), and how does CLL progress? Dr. Matthew Davids details the stages of CLL and indications for when it’s time to treat the condition.
Dr. Matthew Davids is Director of Clinical Research in the Division of Lymphoma at Dana-Farber Cancer Institute. Learn more about Dr. Davids here.
Related Resources:

|
|
Transcript:
Katherine:
Okay. So, how does CLL progress? When do you know when it’s time to treat?
Dr. Davids:
The stages of CLL involve the progression of the disease. When we first meet patients, often they only have cells circulating in the blood, and that’s called stage 0 disease. It’s one of the few cancers where there’s actually a Stage 0 before even Stage I, and the reason for that is that many patients can go for years on Stage 0 disease. But as the burden of the CLL cells begin to accumulate in the body they can start to collect in their lymph nodes, and the lymph nodes can start to swell up whether it’s in the neck or the armpits or elsewhere. That’s stage I disease.
They can accumulate in the spleen, which is an organ in the abdomen. It’s kind of a big filter for your bloodstream, and as the filter traps more of these lymphocytes the spleen can slowly enlarge over time. That’s stage II disease.
And then finally, the CLL cells can get into the bone marrow, which is like the factory for making your blood cells. And if the factory floor gets all gummed up with CLL cells it can’t make the normal red cells, that’s called anemia. Or it can’t make the normal platelet cells, that’s called thrombocytopenia. And when we start to see those more advanced stages III and IV of CLL, that usually does require treatment. And what the treatment does is it clears out the factory floor and it allows for the normal machinery to make the normal blood cells again. So, that’s one of the more common reasons why treatment is needed is due to anemia and low platelets. Second reason can be if the lymph nodes or spleen get so bulky that they’re uncomfortable or threatening organs internally. We want to treat before that becomes a real threat.
And then, the third thing that usually happens as the disease progresses, patients can develop some symptoms, what we call constitutional symptoms. These can be things like unintentional weight loss, drenching night sweats that are happening on a consistent basis, and those sorts of things. So, if that’s happening at the same time as these other factors are progressing, those would be reasons to treat.
And notice that one thing I did not say is the white blood cell count itself.
That’s a common misconception. Some people think that as the white blood cell count goes higher – and people use all different thresholds, 100, 200 – that by crossing that threshold you need to start treatment. And in fact, that’s not the case. We have many patients whose white blood cell count can get very high but then it can kind of level off and plateau for a period of several years, and as long as they don’t meet those other treatment indications, they don’t need to be treated just based on the white count alone.
Should Patients “Watch and Wait” Before Starting CLL Treatment?
Should Patients “Watch and Wait” Before Starting CLL Treatment? from Patient Empowerment Network on Vimeo.
What do chronic lymphocytic leukemia (CLL) patients need to know about watch and wait? Dr. Matthew Davids shares the meaning of watch and wait, when it’s appropriate for CLL patients, and which factors are monitored to ensure the best care.
Dr. Matthew Davids is Director of Clinical Research in the Division of Lymphoma at Dana-Farber Cancer Institute. Learn more about Dr. Davids here.
Related Resources:

|

|
Transcript:
Katherine:
We have a question from the audience. Linda writes, “I’ve heard that CLL doesn’t need to be treated right away. Is that true?”
Dr. Davids:
That is true for the majority of CLL patients, and it’s actually a very counterintuitive thing. We’re conditioned that if you have cancer that it’s important to be proactive and get rid of it as quickly as possible, the sooner the better, and that is actually not the case in CLL. And we didn’t just take a guess that that’s the best approach. This is actually something that’s been studied in clinical trials. There were several clinical trials launched in the ‘70s and ‘80s looking at an early intervention strategy using a chemotherapy-based approach to see if treating at the time of diagnosis would be better than waiting until patients developed more significant symptoms.
And all of those studies did not show a benefit to early intervention.
Now, more recently those studies have been challenged as somewhat out of date, which is a fair criticism because they used an older chemotherapy drug. And so, there is a newer study now going on in Europe that is looking at early intervention with the drug ibrutinib, which is one of our novel agents for CLL, looking to see if early intervention with ibrutinib (Imbruvica), particularly for patients who have a higher risk form of CLL, may be beneficial.
But we have seen some data now already presented from this study that do not show any improvement in how long the patients live by treating with ibrutinib early, and we do see some of the typical side effects that we’re accustomed to seeing with ibrutinib. So, even with the newer data that we’re seeing, we still do not recommend early intervention for patients with CLL.
Katherine:
I’ve heard this term “watch and wait.” What does that mean?
Dr. Davids:
Yeah, it’s not the best term because it’s very passive. That refers to this observation strategy. I like to think of it more as “active surveillance.” It seems more proactive because you’re doing something about it.
You’re really checking the blood counts, you’re getting your physical exam, you’re checking in on symptoms, these sorts of things, and really keeping a close eye on the disease. And that’s the approach that we like to take
with our patients to really keep them engaged, making sure they’re staying up-to-date on their screenings for other cancers, making sure they’re getting vaccinations, these sorts of things are all the things we do with active surveillance.
Katherine:
How is someone monitored during this watch-and-wait period?
Dr. Davids:
It varies depending on individual patients. We’ve alluded to the fact that there’s different genetic subgroups of CLL already, so there are some patients that have higher-risk disease. The example of that usually is deletion 17p that people may have heard of on the FISH test. For those patients I usually am seeing them every three months or so, physical exam, checking on their history, checking their blood work. But there’s quite a few CLL patients who have lower-risk disease. If they have for example mutated IGHV, if they do not have the 17p for example, those patients may be able to be seen once every six months or so with a similar setup.
I don’t routinely get CAT scans on a regular basis for most patients. Most patients don’t need bone marrow biopsy tests unless they’re starting treatment. So, it’s mostly it’s exam, talking to patients, and checking the blood work.
Who Is on a Patient’s CLL Care Team?
Who Is on a CLL Patient’s Care Team? from Patient Empowerment Network on Vimeo.
Who are the members on a chronic lymphocytic leukemia (CLL) patient’s care team? Dr. Matthew Davids explains the members of the healthcare team – and shares advice for ensuring the patient receives complete information for optimal care.
Dr. Matthew Davids is Director of Clinical Research in the Division of Lymphoma at Dana-Farber Cancer Institute. Learn more about Dr. Davids here.
Related Resources:

|
Transcript:
Katherine:
When a person is diagnosed with CLL they have a whole healthcare team. Who’s typically on that team?
Dr. Davids:
It’s definitely a multidisciplinary team.
Usually there’s an oncologist-hematologist who’s leading the team as a physician, but there’s a very large team of other people who are involved, whether it’s an advanced practice person such as a nurse practitioner or a physician’s assistant. They’re often very closely involved with the day-to-day patient care. There’s nurse navigators in some places that can help with getting access to these novel agents and with looking into clinical trial opportunities. There are pharmacy folks who are very helpful sometimes in checking in on side effects, and advising on dosing, and so forth.
That’s more on the provider side of things. But, of course, the care team really includes the caregivers for the patient, whether it’s family members or friends, who are really a crucial part of this. The field is very complicated, and one of the challenges with COVID recently is that I’ve always invited family members and friends to come to visits with patients, because I do think it’s helpful to have many people listening. And that’s been hard because we’ve had to restrict visitors usually to either no visitors or one visitor because of COVID precautions.
Even if that’s the case, you can still have people dial in by phone or use technologies like FaceTime to try to have them there with you, because I think having that extra set of ears can be helpful as you hear all this information coming at you from your oncologist.




