The pandemic has distorted our livelihood and forced many of us into teleworking whether we were willing or unwilling. We’re plastered to our computers not just in the home office, but at our kitchen tables, or on the bed. We find ourselves having to make adjustments on a regular basis. Responsibilities may have been added to your already hefty plate. Your new work environment may not be favorable. Maybe you simply can’t concentrate. We just can’t seem to escape the pings and alerts from work colleagues. Working from home is new to many of us. However, the concept of work-life balance is not. Yet, instead of home being a sanctuary, it has become a boundless environment for work and stress. Through this journey, we can relearn what work-life balance is, and how intervening factors like stress meddle with our body and mind. We can learn the value mindfulness has in creating boundaries that benefit our health and productivity, and be empowered with tools to build and sustain our immunity.
In the moments we’re experiencing stress we don’t stop to think about the effects it can have on our mind, body, and soul. Being overworked, getting familiar with remote working conditions, or trying to make child-care arrangements can be awfully difficult during a pandemic (Harnois & Gabriel, 2002). Stressors such as these can drive workers into depression, cause sleep disorders, body aches and headaches, and lead to other short- and long- term effects. Job-related stress can affect our immune system by lowering our resistance to infections. Brace yourself, we’re about to hop on the science train, but only for a few stops so you’ll be fine.
Who turned off the lights?
Stress flips the switch on the central nervous system causing it to go into defensive mode (Han, Kim, & Shim, 2012). The body reacts in efforts to regain homeostasis or regain balance. As previously mentioned, stress has the ability to cause depression, sleep disorders, body aches, and a lower immune system. Did you know that stress, sleep, and immunity are related (Han, Kim, & Shim, 2012)? Small immune signaling proteins called cytokines aid in regulating sleep. When these proteins fail to perform properly due to stress, this interrupts phases of sleep. When experiencing this stress, an irregularity in the secretion of the hormone Cortisol occurs.
Depression is a common and complex disorder with the ability to affect your daily life including work and productivity (National Institutes of Health, 2016). The hippocampus, amygdala, and the prefrontal cortex are three parts of the brain that seem to have major roles in depression (Cirino, 2017). When we experience depression, Cortisol secretion increases causing chemical imbalances which can lead to the reduction of brain cells (neurons). In a Korean study published in Stress and Health, individuals who experience work-related stress are at a higher risk of experiencing major depressive issues (Lee, Joo, & Choi, 2013). Symptoms associated with work-related stress include a reduction in the ability to concentrate, fatigue, insomnia, and feeling counterproductive.
An increase in proinflammatory cytokine levels can cause inflammation within the body (Leonard, 2010). This can lead to major depression followed by type 2 diabetes and other inflammatory diseases. Cytokines are involved with adaptive immunity and have been linked to COVID-19 infections (Costela-Ruiz, Illescas-Montes, Puerta-Puerta, et al, 2020). Weakened immune responses have been linked to patients with comorbidities. While the available information regarding COVID-19 is ever changing, what we do know is severe pre-existing conditions, including pregnancy, are linked to weakened immune responses placing these individuals at a higher risk of contracting the virus.
Road to Redemption.
Now that we have a better understanding of stress, learn to set your boundaries to alleviate it. Establish boundaries in all aspects of your life, especially with work. This ensures that your needs and your health are placed at the forefront. Think of them as safeguards for yourself. As difficult as it may be to establish them, understand that they are without question essential for your efficacy in and out of work. Working without boundaries is when stress raids the mind, body, and soul creating an imbalance. Here are a few practices to reclaim your balance: be mindful, create a workable workspace, listen to your body, reevaluate your time, say no.
Being mindful is having that ability to find calm in times of chaos. Be conscious and aware of the moment, relax, and BREATHE. Only you are in control of you. This is a type of meditation that can be implemented in your daily life at any moment. Let’s take a few moments to practice. Stop what you’re doing, turn off the TV, put your laptop to the side, get comfortable, and gently close your eyes. Take a deep breath in, then slowly exhale. If you hear noises, leave them be, continue to breathe. Do this for about 5 minutes. This practice is to help you find your calm, clear your mind, and become hyperaware. This method of nurturing your mind and body has the ability to mitigate stress, anxiety, improve sleep, and improve attention (Mayo Clinic, 2018). There are many practices for mindfulness which can be found on the Complete Guide to Mindfulness.
We are no longer in our offices or confined to our cubicles so we must create workable workspaces, and implement our boundaries. Yes, your new comforter was just shipped from Amazon, but allow the bed to be a place for rest not work. Create a space to enhance productivity yet allow comfort. Here are tips to transform a section of your home into a conducive workspace:
1. Invest in a quality chair and desk/or small table
- Maintain good posture. If you feel yourself slouching, readjust or move around We want to avoid body aches, so listen to your body. Be aware of its needs.
2. No desk?
- Use the kitchen table or counter, a coffee table (make sure you have some sort of back support).
- If you must use your bed because your room is the only place of silence, ensure your bed is made. Sit on top of your new comforter with your back against the headboard
3. Good lighting is a must.
4. Keep your workspace organized using bins and folders
- Disorganization is distracting, limits movement, affects motivation, reduces your performance, and shows lack of control (Roster & Ferrari, 2019).
5. Do not let work leave your workspace. The rest of your home should be designated a non-working area.
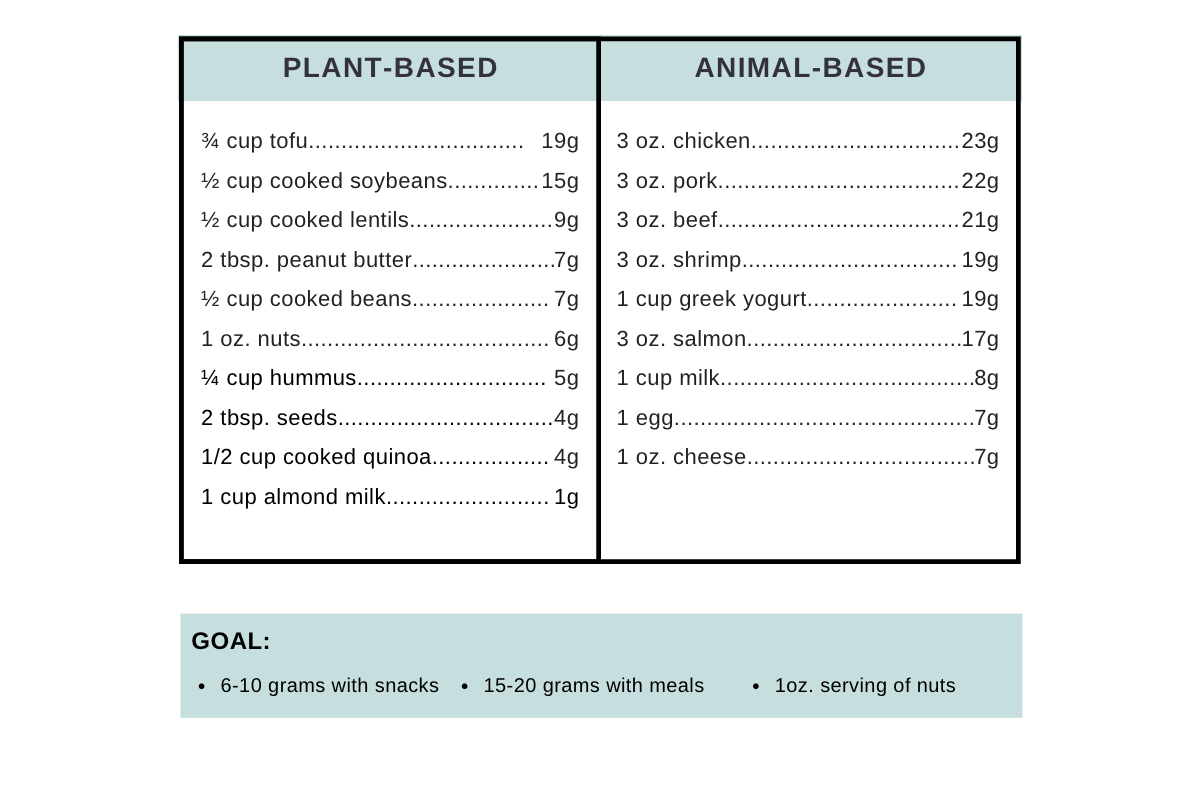
Listening to your body is an aspect of creating boundaries. Do not let work interfere with your health. Know when to get up to stretch, grab water, have a snack, or take lunch. If you must, inform your team of the time you will take lunch daily. Having good nutrition is the first thing that will ensure we’re energized and healthy. Instead of ordering something to go for lunch, try meal prepping. Use Sunday as the day to prepare and organize your meals for the week, including your snacks.
Restock on the elderberry! Since we’re all being hyperconscious of where we venture in the world, incorporate things to boost your immune system such as Emergen-C and elderberry. Elderberry is a substance extracted from the elder tree which many use as a dietary supplement to help boost their immune system. It can be consumed in the form of syrup or even gummies. Disclaimer, before the use of any dietary supplement it is best practice to consult your healthcare provider.
Reevaluate your time. You may find that during this time you have accumulated more than 40 hours a week. It’s fine to work additional hours sometimes, but this takes away time from caring for yourself. It interferes with your work-life balance. Although we’re home, this shouldn’t equate to extra time to tap on computer keys. Reevaluating your time takes a level of mindfulness to understand the importance of taking care of you: your mind, your body, your soul.
Saying no can be difficult, especially to a loved one or your boss. However, you should listen to your mind, be aware of what you are capable of, and respect your time. Knowing when to say no in some respects may be less difficult than others. Saying no is powerful. It is the ultimate boundary we can create for ourselves and it is okay.
Our fight with this global pandemic has yet to near the end. If we are equipped with the tools to tackle our stress and adjust as needed, we may be equipped to continue our lives teleworking. We have learned to understand the deteriorating effects stress has on our health. It can disrupt sleep patterns, make us susceptible to depression, and weaken our immune systems. Each one of these conditions are tightly tied together by stress which we must keep unbound. However, the tools to reclaim our balance will aid us in this situation. Being mindful, creating the awareness we need to breathe and focus for productivity in work and life, will assist us in creating needed boundaries. Whether these boundaries are centered around a conducive workspace, listening to our bodies, reevaluating our time, or simply saying no, it is a necessity to properly control and lessen the amount of work-related stress we experience in these crucial times.
References
Cirino, E. (2017). The effects of depression on the brain. https://www.healthline.com/health/depression/effects-brain#1
Costela-Ruiz, V. J., Illescas-Montes, R., Puerta-Puerta, J. M., Ruiz, C., & Melguizo-Rodríguez, L. (2020). SARS-CoV-2 infection: The role of cytokines in COVID-19 disease. Cytokine & growth factor reviews, S1359-6101(20)30109-X. Advance online publication. https://doi.org/10.1016/j.cytogfr.2020.06.001
Han, K. S., Kim, L., & Shim, I. (2012). Stress and sleep disorder. Experimental neurobiology, 21(4), 141–150. https://doi.org/10.5607/en.2012.21.4.141
Harnois, G. & Gabriel, P. (2002). Mental health and work: impact, issues, and good practices. https://www.who.int/mental_health/media/en/712.pdf
Lee, J., Joo, E., & Choi, K. (2013). Perceived stress and self-esteem mediate the effects of work-related stress on depression. Stress and Health, 29(1), 75–81. https://doi.org/10.1002/smi.2428
Leonard B. E. (2010). The concept of depression as a dysfunction of the immune system. Current immunology reviews, 6(3), 205–212. https://doi.org/10.2174/157339510791823835
Mayo Clinic (2018). Mindfulness exercises. https://www.mayoclinic.org/healthy-lifestyle/consumer-health/in-depth/mindfulness-exercises/art-20046356
National Institute of Health (2016). Depression basics. https://www.nimh.nih.gov/health/publications/depression/index.shtml
Roster, C., & Ferrari, J. (2019). Does Work Stress Lead to Office Clutter, and How? Mediating Influences of Emotional Exhaustion and Indecision. Environment and Behavior, 1391651882304–. https://doi.org/10.1177/0013916518823041
India is interested in government policies and regulations regarding clinical research and mental health. She is a member of the HEET (health equity emissary team) , a health equity education and awareness channel committed to spotlighting health disparities impacting vulnerable populations.