Quick Guide to Health Insurance Options
This guide was originally published by our partner, Triage Cancer, here.
2021-Health-Insurance-Options-Quick-GuideThis guide was originally published by our partner, Triage Cancer, here.
2021-Health-Insurance-Options-Quick-Guide
What are some of the barriers to clinical trial participation? What is a virtual clinical trial? Should my doctor be speaking to me about my clinical trial options? Dana Dornsife, founder of Lazarex Cancer Foundation, speaks to the key barriers in trials and how COVID-19 has really opened the door for a lot of opportunity to engage with patients around clinical trials.
Barriers to Clinical Trial Participation from Patient Empowerment Network on Vimeo.
What is a Virtual Clinical Trial? from Patient Empowerment Network on Vimeo.
COVID and Clinical Trials: Has There Been a Shift? from Patient Empowerment Network on Vimeo.
From PEN-Powered Activity Guide V, beloved medical oncologist Dr. Bora Lim of The University of Texas MD Anderson Cancer Center walks us through what a clinical trial is, the phase of how drugs get approved, and how the pandemic crisis has amplified the criticality of clinical trials.
What is a Clinical Trial? from Patient Empowerment Network on Vimeo.
How Do Drugs Get Approved? from Patient Empowerment Network on Vimeo.
Will Pandemic Transform Future of Clinical Trials? from Patient Empowerment Network on Vimeo.
Clinical Trials as an Empowerment Tool from Patient Empowerment Network on Vimeo.
There are two ways to fight cancer, both of which are equally as important. The first is physical and the second mental. Journaling might not be able to help with the physical symptoms, but easing the mind can truly help in such situations.
By providing a safe place to store your thoughts and experiences, you will be able to find a great source of power. If you have never thought about journaling before, this might be the perfect time for you to give it a try. Here are some important reasons why this might be a very great decision.
Some people believe that battling cancer is only filled with negative moments and experiences. While that is true to a big extent, there can be plenty of memorable moments that you might want to keep track of. The beginning of your treatments is a moment that you can write about and think about when this situation is over.
Other important moments might include family gatherings, important presents you might receive, very bad and very good days that stand out in your treatment course. Just because a day way difficult doesn’t mean it should be considered bad. At the end of this difficult journey, you will be able to look back at everything you wrote and remember the good and bad times.
Another great reason why journaling can truly help cancer patients during their treatments is because of symptom management. Research has actually shown that journaling can help with combating symptoms and dealing with the physical size of things.
Writing about how you feel and what you are going through can help you sleep better and feel more energetic. Getting plenty of rest will allow you to feel less nauseous, be in a better mood and battle everything with a stronger will. The more you face your symptoms, the stronger you will feel through your treatment.
The stress that can be caused by such a difficult diagnosis is great and can truly affect your mood and outlook on life. Being under stress can make you feel tired, mess up your sleeping schedule and make you feel more negative about everything. This is not ideal for any situation you are in in your life and there are ways to overcome it.
Journaling can provide you with a safe space to write everything you have in your mind. During your treatments, you will possibly want to appear strong in front of your family and you might not want to share everything you feel. You can write all your thoughts in your journal and let everything out. This way you will be able to handle everything you face and feel a lot less stressed.
When dealing with any hardship in life, it is important to keep thinking of things that bring you joy. Journaling has helped me create a notebook full of memories, which I can go through any time I need some positivity in my life. You don’t only have to put words into it but anything and everything that makes you think of memories and people you hold dear.
In your journal you can keep stickers, receipts, drawings and cards from loved ones. Then you can write how receiving these things made you felt. When the days get difficult and you are struggling, open your journal again. Read through everything nice you have collected and it can help you remember all the reasons why this difficult process is worth it.
Last but not least, another important reason why journaling is so helpful during cancer treatment is that it can help keep track of your progress. There are going to be many days that will be hard and many that will be good and filled with hope. In order to be able to go through both, it is important that you keep track of everything new that happens in your journey.
The good days will help you remember that things will get better. The difficult days will allow you to live in the moment and work on staying positive. Journaling this experience can also help your family better understand what goes on in your head and how they can help. After you have successfully put this difficult period of your life behind, you can even share your story with other patients through your journal.
Journaling is a creative and fun activity that can help you deal with certain symptoms and negative thoughts during your treatment. Even if you have little experience with writing, journaling gives you the chance to get creative. You don’t need any special skills in order to journal. You just need a notebook, some fun colors and a few thoughts in your head.
Through writing about your experiences, you will be able to express how you feel and let everything run its course. This treatment course might be tough, but writing everything down will help you see just how much progress you are making. This can truly help you feel stronger mentally and physically and overcome this situation like a true warrior!
Bridgette Hernandez is a professional writer and editor for Subjecto. She loves helping her audience find
new ways to incorporate writing into their daily lives in order for them to overcome many different
difficulties. This is why she often teams up with different platforms to help spread this exact message. In
her spare time, Bridgette loves to read and spend time in nature.
Getting a cancer diagnosis can easily be the most terrifying, heart-wrenching experiences one has in their lifetime. Everything from different treatment options (if you’re lucky), to financing, and maintaining quality of life suddenly are in full force front and center. It can be hard to know who to turn to if you’re not directed to a support group (of which there are many), and especially how to tell loved ones and co-workers. The choice is yours, of course, in whom you wish to tell and when – there is no right or wrong answer. (However, I and many others have found that having a caregiver to help manage appointments, billing, etc. can help).
Should you choose to tell others, here are some tips that I have read and/or heard from other cancer patients/survivors as well as some I have found personally helpful:
Carly Flumer is a young woman who was diagnosed with stage I papillary thyroid cancer at the age of 27. She recently received her Master’s degree from Boston University in Health Communication and received her Bachelor’s from George Mason University in Health Administration and Policy. While being diagnosed with the “C” word at such a young age was a surprise, as it would be to anyone, she found strength, support, and inspiration in sharing her cancer journey on social media. As a result of her health outcome, she looks to advocate for other cancer patients through education, research, and health literacy.
At a time when health is top of mind for everyone, despite the stressors, how can we ensure to emerge emotionally, physically and mentally resilient? Patient Empowerment Network Care Partner Manager, Sherea Cary sits down with distinguished guests, Sara Goldberger and Dr. Shivdev Rao to discuss building resilience and boosting immunity. Both experts define resilience, provide tips for boosting heart-lung health and provide useful tools for cultivating resilience.
Defining Resilience from Patient Empowerment Network on Vimeo.
Tips for Boosting Heart and Lung Health from Patient Empowerment Network on Vimeo.
Community Resources and Tools for Cultivating Resilience from Patient Empowerment Network on Vimeo.

Sara Goldberger, MSSW, LCSW-R, has been an oncology social worker for 30 years. Currently she is the Senior Director, Program for the Cancer Support Community Headquarters. She has also worked in hospitals and community NFP settings. She is a member of several Advisory Boards is a frequent presenter and author. As AOSW strives to continue to advance excellence in psychosocial oncology, Sara hopes to play a part in efforts to educate, advocate, develop resources, expand on research initiatives, and create networking opportunities so that AOSW can improve the care of people impacted by a cancer diagnosis.
These days, whether you’re spending more time there or you need a place to unwind after a long day, you need to feel like your home is your happy place. With the help of a few simple tips you can turn your home into your very own sanctuary.
Think about where and when you feel the most comfortable and happy; then bring elements of that into your space. Whether you feel your best reading under a cozy blanket and low lighting, or painting in a sunlit room, consider your needs for the space. It doesn’t have to be complicated, says Professional Organizer Kristy Potgieter at KLP Organizing, LLC. Her philosophy is: simple is better.
Sound, smell, and color can all evoke emotions. Play music that soothes you or makes you happy, use candles, oils, or incense to fill your space with your favorite scents, and paint your walls with neutral or calming colors. Even changing out your light bulbs can make a difference. Pink light bulbs give a warm, calm glow to your space.
Clutter causes anxiety and stress so your best bet is to get rid of it. While clutter looks different to everyone, a good rule of thumb is to remove anything that doesn’t serve a purpose or make you happy. For the things you use on a regular basis, Potgieter recommends storing them in baskets and bins, which can be both decorative and functional. She also says keeping your kitchen counters clear is a simple way to make your home appear clutter-free.
You can place a vase of fresh-cut flowers on your table or bring in some house plants. If you don’t have a green thumb, a photo of the ocean, a wall painted green, a water fountain, some seashells, or a piece of wood are all okay ways to incorporate nature into your home. It can be as simple as opening a window and letting in the sunlight, which is a known mood booster.
You don’t have to ban technology altogether, but pick times, such as during meals and the hour before bed, to not use technology at all. Spend less time on social media platforms by deleting the apps on your phone and only using your computer to log onto those sites. You can also use the “do not disturb” settings on your devices to allow yourself some down time.
Whatever you do, remember Potgieter’s philosophy and keep it simple. Address the things that are most important to you and let the other stuff go. “The first thing I think of when making a home a sanctuary is really taking a look around and making sure all the things you see are things you love,” she says.
Jennifer Lessinger is a professional writer and editor who learned the value of patient empowerment during her struggle with a hard-to-diagnose and complex endocrine disorder.
Resilience is our capacity to bounce back from the inevitable challenges of being alive. When challenges arise, our meandering minds can take us into various worrisome directions, leading to a host of negative emotional states and their subsequent adverse effects on our well-being.
Although we may not have control over the external factors in our lives or needless to say our genetic predispositions, we do have the capacity to cultivate inner psychological faculties that enable us to weather the storms of life with relative calm. For most of us, these internal resources are underdeveloped. They require intentional cultivation through the regular practice of actions that support their development. Among these inner resources are self-awareness, self-acceptance, and a secure inner base to fall back on.
What is Resilience? from Patient Empowerment Network on Vimeo.
Anchoring the Mind from Patient Empowerment Network on Vimeo.
Focusing the attention on the natural breathing process and body cultivates self-awareness and tends to have a calming effect on the mind. By doing so non-judgmentally, we accept the process as it is truly experienced. This is not an advocation of apathy towards our lives. To the contrary, by shining the light of awareness on our experience and accepting it as it truly is, we are given a clarity from which to make any necessary course corrections in our lives.
Awareness of Breath from Patient Empowerment Network on Vimeo.
Awareness of Body from Patient Empowerment Network on Vimeo.
A secure base is supported by continually returning our attention to our breath and body when distracted by the meandering nature of the mind. By regularly practicing the activities here offered you can enhance your capacity to bounce back and calmly weather the fluctuating trials of life.
Broderick Rodell has a PhD in chemical engineering from the Georgia Institute of Technology and a Doctorate of Naturopathic Medicine from Bastyr University. His search for self-betterment led to his passion for mindfulness. He considers himself a dedicated student and practitioner of yoga including contemplation, meditation, breath work, and mindful movement. Broderick believes that through individual evolution we can all tap into greater possibilities within ourselves.
“There’s something to be said for not being a patient,” one of my doctors said.
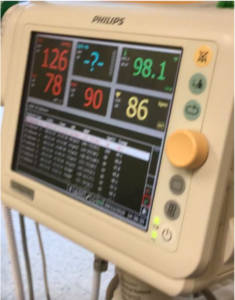 “It feels so good,” I said during our telemedicine appointment, “to be away from the hospital for eight weeks in a row.” It’s the longest hospital break I’ve had since being diagnosed with cancer last summer. Before mid-March, I’d been to four to ten medical appointments every month. Being a cancer patient felt like a full or half time job. Because of the pandemic, I’m now treated by my oncology team from the comfort of my own home.
“It feels so good,” I said during our telemedicine appointment, “to be away from the hospital for eight weeks in a row.” It’s the longest hospital break I’ve had since being diagnosed with cancer last summer. Before mid-March, I’d been to four to ten medical appointments every month. Being a cancer patient felt like a full or half time job. Because of the pandemic, I’m now treated by my oncology team from the comfort of my own home.
I don’t miss shuffling from room to room or floor to floor and sitting in waiting rooms for hours. I love not needing to ask for rides or take cabs or public transportation while my white counts are low. I don’t miss being poked, prodded, weighed, and measured or having my vital signs documented in hallways while removing my coat, wig, and shoes. I love not having to roll up sleeves for the vials of blood to be drawn or to pull down my pants so the doctor can put a stethoscope to my belly and bowels.
Because of the increased health risks at hospitals, new access to telemedicine, and flexibility around clinical trial protocols, I can see my oncologist, face to face, through Zoom. Questions can be answered ,via email, a text, or a phone call. Clinical trial drugs are overnighted to me.
I enjoy the time and money I’m saving and the convenience of getting all care from home. But I also miss the real-life hugs, handshakes, and high fives that used to come with seeing the clinical team in person.
Many cancer patients are losing jobs, homes, loved ones, and health insurance. For those newly diagnosed with cancer, surgery, scans, and treatments must be done all alone. Those in active treatment are often terrified of catching COVID-19 while immunocompromised. Others are afraid hospital visits will expose our family members to COVID.
It’s startling how much hospital protocols and procedures have changed. When I look back or think about what comes next, I worry. I hope the pictures and stories below capture what it’s like to be an oncology patient and how swift and severe the COVID-related changes over the last few months have been and continue to be.
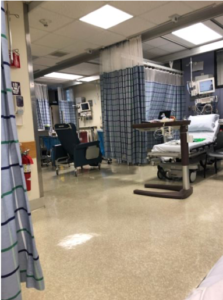 My partner drove me to the hospital on the morning of my surgery. We checked in before 6a.m. and waited, with others, in the lobby.
My partner drove me to the hospital on the morning of my surgery. We checked in before 6a.m. and waited, with others, in the lobby.
Eventually, we were called up and walked, single file, through halls by someone escorting us to the pre-op area. Each one of us was assigned a bed (pictured) and a nurse (not pictured). The photo is of the pre-op area.
My partner got to visit me before surgery. He was there when the surgeon, nurses, fellows, and anesthesiology came to prepare me for surgery.
If surgery were scheduled today, my partner wouldn’t be able to stay with me.
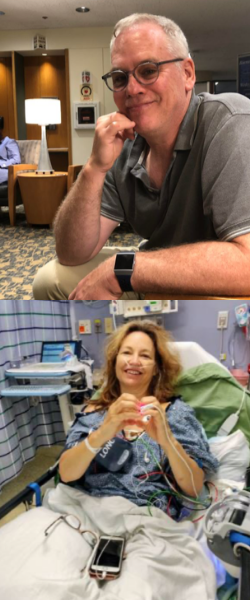 This is me in post-op. My partner took this photo on his phone and was able to share it with my family and friends to let them know I made it through surgery. They were worried because it went hours longer than expected.
This is me in post-op. My partner took this photo on his phone and was able to share it with my family and friends to let them know I made it through surgery. They were worried because it went hours longer than expected.
In the photo, I’m high as a kite and happy to be alive. I’ve just downed the iced coffee my partner snuck in (as planned and with permission from the nurse). In the photo, I am still in shock that my surgery was five hours long, it’s afternoon, and that cancer was found. I don’t yet know how serious my diagnosis will be. That will come twelve hours after surgery when the surgeon explains my cyst was actually a cantaloupe-sized cancerous tumor, aggressive, advanced, and usually chronic. Mercifully, my partner is with me as she explains that she had to do a total hysterectomy, removing ovaries, fallopian tubes, lymph nodes, and my omentum and lays out the timeline for chemotherapy.
My partner held my hand and crawled into my bed to hold me while I sobbed. But he provided far more than essential emotional support. He helped me stand and keep my balance, helped me get to my first trip to and from the restroom. He was there to advocate for me when I dozed off and to get the nurse when my call button went unanswered. He was the one who provided my loved ones with updates. He was the one who snuck my favorite health foods to help “wake up” my digestion enough to allow me to be discharged after one day.
It’s hard to imagine what that traumatic and challenging day would have been without him. I can’t imagine recovering from major surgery and receiving such devastating news alone but it’s what many diagnosed with cancer during COVID now endure.
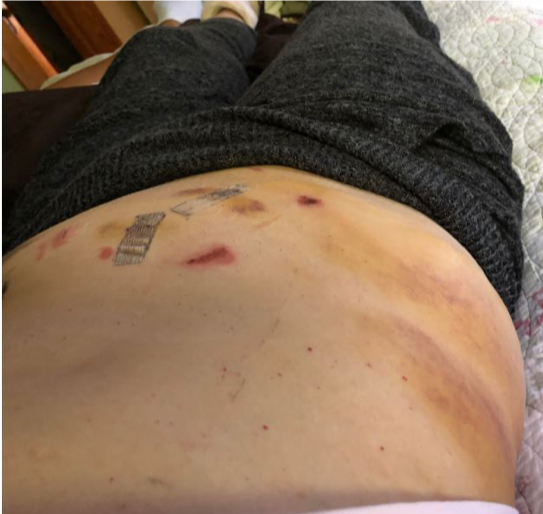 Going home after surgery is comforting and scary. My right leg was giving out from under me because my obturator nerve “got heat” during my surgery. I had trouble standing in the shower or lifting my right leg onto the bed or into a car. I had extensive swelling and bruising on my right side and pelvic area and had a bit of a reaction to the bandage tape. I didn’t know what was normal. And after a phone call to the hospital, I was asked to come back in for a check-up.
Going home after surgery is comforting and scary. My right leg was giving out from under me because my obturator nerve “got heat” during my surgery. I had trouble standing in the shower or lifting my right leg onto the bed or into a car. I had extensive swelling and bruising on my right side and pelvic area and had a bit of a reaction to the bandage tape. I didn’t know what was normal. And after a phone call to the hospital, I was asked to come back in for a check-up.
Today, I’d either have had a telemedicine appointment or need to decide if an in-person visit with a medical professional is worth possible exposure to COVID. These are the types of decisions we are all facing but it’s especially scary when one is already vulnerable and fighting for life.
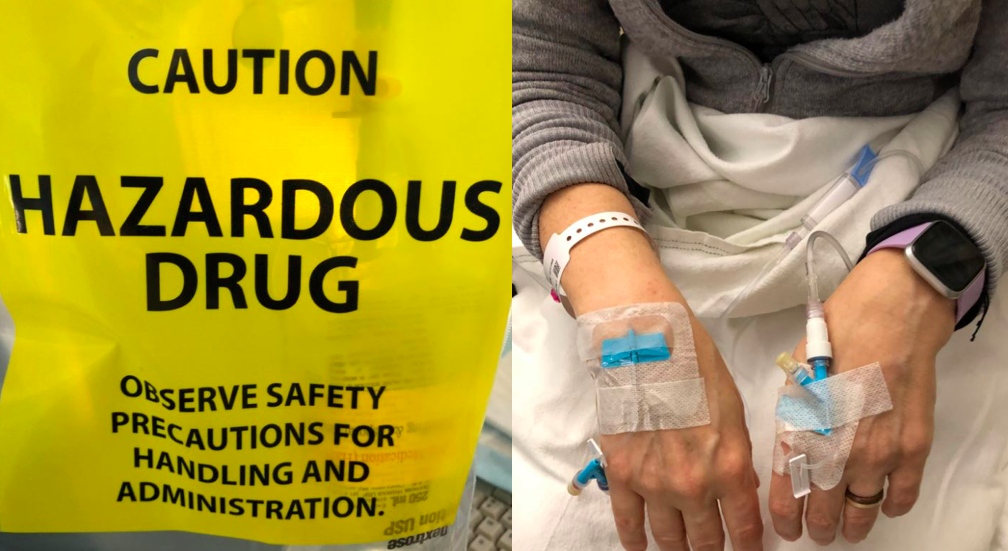
Getting chemotherapy infusions is time-consuming, scary, and intense. Everyone reacts differently to the many drugs given with chemotherapy (such as Benadryl, steroids, Pepcid, and anti nausea drugs). Everyone reacts differently to the chemotherapy, marked hazardous, that require the nurse to wear gloves, masks, and protective clothing to prevent contact in case of accidental spills. Some drugs make you sleepy, and parts of your body numb. Others make you feel amped, wired, and agitated.
Some cause nauseous, headaches, or allergic reactions, immediately and others not for days or weeks.

Having a chemo-buddy like Beth was a huge help. She was the one who asked for window seats in the infusion center, who made sure I got warm blankets. She massaged my feet and reminded me to listen to guided imagery. She sat with me in waiting rooms as we waited for my labs to come back to make sure my white and red blood counts weren’t too low, my liver counts not too high, and that the chemo was making my tumor marker scores go down.
She was the one who touched the elevator buttons for me, the one who walked me to the car and handed me off to my fiancé at the end of the day. She was the one who got me water, coffee, or snacks.
I felt safer whenever I had a chemo buddy with me and Beth would also take notes and make sure I didn’t skip any of my questions just because the oncologist seemed in a hurry.
Beth was not only a source of support but provided an extra pair of hands to plug in my iPhone, to hold my bags, food, or books. She was the person I could share tears, laughs, and heart to hearts with. She listened as I worried about my daughter, as I struggled to balance work and parenting.
She was there to support me as I talked endlessly about healthy eating, fasting, supplements, and complementary medicine. But the greatest comfort of all was knowing she would be there if passed out, fell, or had an allergic reaction to all the treatment drugs. At my last treatment, I was alone and Beth at home. It was hard.

Social distancing during treatment is hard even for introverts like me who need a lot of alone time. When physically weak, short visits with loved ones who bring food, hugs, and gifts are life-affirming and life-changing.
Those who show up do so for cancer patients as well as our families. They help us to take care of our kids, partners, pets, plants, and housework. They help us manage as we face fear and loss, whether losing jobs or body parts, or hair and having few or no visits is hard. Today, barber shops where we might get our heads shaved are closed.
The wig shops and stores we go to for hats and head coverings are often closed.

We can’t go out to eat with loved ones, or do yoga on good days. We can’t have parties for our loved ones to create normalcy or new rituals. We can no longer go out in the public either. We can’t do things such as sitting alone writing in a journal and drinking a smoothie when swallowing food is too hard.
We can’t travel to remind ourselves there is still beauty and magic in the world and to enjoy our loved ones and lives as much as possible.
These are not all small things or luxuries in coping with the brutal effects of cancer treatment and chemotherapy. They can change the cancer and recovery experience and all that helps keep us strong.
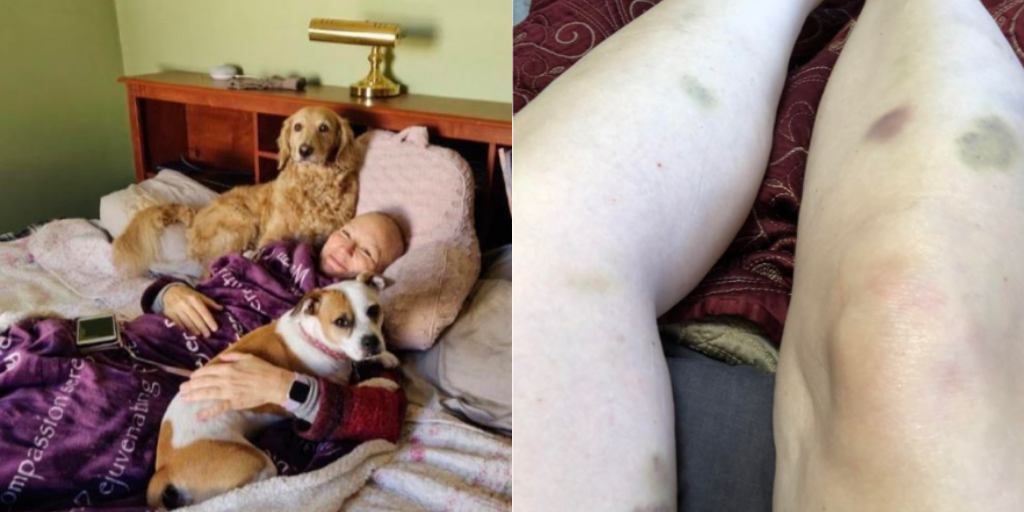
We need others when we are sick. We might need help standing, walking, or eating. We might need rides, treatments, or blood or platelet transfusions. We might need help articulating symptoms and side effects. To have fewer in-person visits when so medically vulnerable can be anxiety-producing.
We also have less in-person celebrations with our clinical teams when we finish a line of chemotherapy or have a cancer-free scan. We no longer have informal pet therapy either with the cheerful and cuddly animals of friends, family, and neighbors.
I can’t imagine going to chemo alone, depleted, and with low white counts.
The increased risks, vulnerabilities, and lack of human company and tactile comforts feels indescribably epic.
My immunotherapy infusions (or placebo) have been put on hold for the past two cycles. I asked if I could remain in my clinical trial if I refused to come to the hospital for treatment until the risk of getting COVID is decreased. Luckily, I’ve been allowed to stay home. Clinical trial protocols, in general, are much more flexible as a result of the pandemic. My medication (or placebo pills) are mailed to me. Before March, in-person prescription filling was required and always took hours.
However, I’ve been weighing what I’ll do if I have to weigh virus-related risks against the possible benefits of clinical trial treatment. If I’m required to be treated at the hospital I may drop out of the trial. This is one of the many difficult decisions oncology patients often face but it’s made more complicated because of the coronavirus. .

The losses, challenges, and changes are worrisome and real. That said, not all the COVID-related changes for oncology patients are bad. The whole world is wearing masks, staying home, socially distancing, and worrying about health, wellness, death, and dying.
Instead of being stared at when I wear a mask, I’m now in good company, because much of the world is doing the same. Many of us are consumed with health issues and worried about health, mortality, and immune functioning.
To be reminded, once again, that health and life aren’t guaranteed to anyone, that we are all facing mortality, and must appreciate every day we have, is strangely comforting. While I’m reminded of our collective vulnerability, to hear health concerns, risks, and challenges confronted as the world and nation’s collective concern is a reminder that none of us are being personally picked on for failing at being human, we are just, in the end, all excruciatingly fragile and mortal.
“I feel like I’ve been slow-dancing with death since last summer but now I feel less alone,” I told my friend Kathy. “It’s like others have joined you on the dance floor,” Kathy said. “Yes,” I said, which once again makes me feel like a person rather than a patient and there’s something to be said about not being a patient….

When not recovering or coping with her recent ovarian cancer diagnosis, chemo brain, and the other treatment-related side effects, Christine “Cissy” White works as Community Manager of the Parenting with ACEs community on ACEs Connection and blogs at www.healwritenow.com. White has been published in The Boston Globe, Spirituality and Health, Ms. Magazine, The Mighty, To Write Love on Her Arms, Elephant Journal, the Center for Health Journalism, and ACEs Too High. She is the 2019 recipient of the Touching Trauma at Its Heart Award, given by the Attachment Trauma Network for her work advocating on behalf of families coping with traumatic stress from developmental trauma. White has led Parenting with ACEs, Parenting After Trauma, and Writing to Heal workshops and speaks passionately about the need for first-person perspectives and the power of lived expertise. Her survivor-led advocacy has been written about in The Atlantic, Huffington Post, and The Mighty.
Since the 1980s, doctors have tried to describe the stages cancer survivors normally go through. Most divide them into a version of the three stages described below:
Acute Survival (Living With Cancer) – Covers cancer diagnosis and any subsequent treatment. During this time, patients will undergo treatment and may be invited to participate in a clinical trial to study new cancer treatments. Sometimes services are offered to patients and their caregivers to address emotional, psychological and financial problems.
Prolonged survival (transient cancer): Post-treatment period during which the risk of recurrence is relatively high. Many patients are relieved that treatment has ended, but are concerned that they will not visit the oncologist regularly. During this stage, patients often visit the oncologist two to four times a year, depending on their circumstances.
Permanent survival (living after cancer): survival after treatment and long-term. Although two out of three survivors declare that their lives have returned to normal, a third affirms that they continue to have physical, psychosocial or economic problems. During this stage, most survivors are cared for again by their GP. Ideally, they have developed a long-term follow-up plan with the oncologist for their regular doctor to implement.
In addition to the physical effects of cancer, survivors experience psychological, emotional, and spiritual consequences. Many of them affect quality of life and can manifest many years after treatment. Here are some of the most common problems cancer survivors face:
Many survivors live in fear that the cancer will return at some point. In some cases, a major event, such as the anniversary of the diagnosis or the end of treatment with the oncologist, can trigger these feelings. Fear can be good if it encourages you to discuss your health changes with your doctor, but it can also cause unnecessary worry. Knowing your own body will help you distinguish between normal changes and more serious symptoms.
Grief is the natural result of loss. In cancer, losses refer to health, sexual desire, fertility, and physical independence. To overcome your pain, it is important to experience all of these feelings. Support groups and psychological assistance can help you deal with these problems.
It is estimated that 70% of cancer survivors experience depression at some point. Depression can be difficult to diagnose in cancer survivors, since the symptoms are very similar to the side effects of cancer treatment, such as weight loss, tiredness, insomnia, and inability to concentrate. In a 10-year follow-up study, symptoms of depression have been found to be associated with shorter survival, so seeking treatment for depression is essential.
Cancer survivors who have suffered amputations, disfigurements, and loss of organs such as the colon or bladder often have to overcome their problems to relate to themselves and to others. A negative body image and low self-esteem can affect the survivor’s ability to maintain relationships with their partner, which will have important consequences on their quality of life. Good communication is essential to maintain or regain intimacy after cancer. Consult a doctor if problems persist.
Many survivors feel that life takes on new meaning after cancer and renew their commitment to certain spiritual practices or organized religion. Research indicates that spirituality improves quality of life through a strong social support network.
Some people feel guilty about surviving cancer when others don’t. You may be wondering “Why me?” Or reevaluate your goals and ambitions in life. If you have a prolonged feeling of guilt, a psychotherapist, a member of the clergy, or a support group can help you express your feelings.
Possibly the biggest challenge cancer survivors face is how others react to their disease. Friends, coworkers, and family members may feel uncomfortable when discussing the diagnosis of cancer. They can keep silent, avoid you, or pretend that nothing has happened. Others may use humor to try to distract you and not think about your situation, instead of offering to talk about your problems. Cancer can be a long-lasting disease, so it is essential to overcome communication barriers.
Social and professional reintegration can be accompanied by many fears: concern about being exposed to a higher risk of infection, lack of enough energy to reach the end of the workday and anxiety about not being able to think clearly due to the so-called “neurological impairment by chemotherapy “or memory loss. In overcoming a life and death situation, many cancer survivors feel alienated from people who have not had the same experience and turn to other survivors for support and friendship.
You may be reluctant to reveal to your bosses and colleagues that you are receiving cancer treatment for fear of being treated differently or even losing your job and health insurance. This creates an atmosphere of uncertainty that contributes to emotional stress. Again, honest communication with your colleagues will help you overcome these feelings.
About the author: Diane H. Wong is copywriter at write essay for me service. She is also a professional nutritionist and plans to start her own blog to share her knowledge with others.
“Is there a pressure to be positive all the time?” my friend Kathy asked.
It’s a good question. I said, “No,” and then “Yes,” and added in a “Maybe.”
But it’s not a simple yes, no, or maybe. It’s actually Yes-No-Maybe all at the same time. My kid is on Facebook and so is my family. My friends are on Facebook and they want the best or at least to know I’m not suffering. I’m aware of that and of them. But that doesn’t mean I show up fake or put on fronts. I don’t.
The pressure to be positive isn’t external. I am safe to be real with SO MANY people and that luxury is a gift beyond measure. The desire to be positive comes from within but it’s not motivated by pressure. It’s real. In general, I ACTUALLY FEEL positive.
And also, when my oncologist asks how my partner or daughter are doing, I say:
“Well, I’m cranky, lethargic, have chemo-brain, and obsessed with recurrence so that’s fun for them…”
That’s also real.
Real is positive.
So, when people say I’m strong, a rock star, a warrior, and a fighter, I can’t say I feel I am any of those things. My day to day to life has been changed and though I feel 100% half-ass as a mom, partner, friend, relative, and employee – I also know I’m doing the best I can.
I don’t even have much time to think of how I’m doing because I’m so busy doing, if that makes sense.
It’s like I woke up after surgery standing in the middle of a highway I didn’t drive myself on. The focus is dodging the cars going 75 m.p.h. on my left and right while feeling groggy and confused. When I manage to make it to the sidewalk or the rest area, the relief I feel is real. I’m happy to be alive and out of danger. It’s a genuine and consuming experience. I’m relieved any time I’m not in the road and also aware I could be dropped back on that highway in another minute, day, week, or year.
That’s the complexity and reality of living with cancer (#ovarian, high-grade serious, stage 3) that, even when it’s effectively treated, still recurs 75% to 85% of the time. To have no evidence of disease isn’t the type of blessing I’ve been in the habit of counting.
For decades, I have had the luxury of physical wellness and had never stayed overnight in a hospital. Health isn’t something I take for granted anymore but that doesn’t make me a warrior as much as it makes me someone changed by cancer more than by choice.
I used to think people were sick with cancer, and either mounted a “successful” fight and returned to living or lost “the fight” and died. It seemed either/or and as those were the two extreme outcomes.
I knew my mother HAD cervical cancer in her early 20’s and survived. I knew that my Nana and her two siblings had cancer in their 60’s, and did not. They died.
I know cancer is always a full-on fight for the person with cancer and those that live with and love them (us), but fights are won or lost and that is the problem with the “fight cancer” narrative. It’s way too simplistic for the complexity of cancer, cancer treatment, cancer survivorship, palliative care, and grief.
It omits the vast amounts of time that many of us live with cancer. We live with it in active form, or in remission, or in fear of recurrence, and sometimes with recurrence after recurrence. That way of living may last one or two years or one or two decades. We may have years we seem to be “winning” the fight and years we seem to be “losing.”
But winning and losing is far too simplistic. Some live and have loss. Some die and should be counted as winners.
I’d never known some fight the same cancer repeatedly, or “beat” it before getting another kind and another and another. I didn’t know that people cancer can be a lifelong disease and that some kinds are genetic time bombs in our bodies and families that can put us at risk even if we never smoked.
I didn’t know that one can have or five surgeries, that the side effects can start at the head (loss of hair, headaches, chemo brain, no nose hair, dry mouth, hearing loss), for example, and go all the way to the feet with lymph edema, joint pain, neuropathy, and that all the organs in between can be impacted as well.
I didn’t know that most cancer side effects are not from cancer but the treatments to fight, eradicate, and prevent more cancer.
I didn’t know that in addition to chemo, one might contend with liver or kidney issues, with high or low blood pressure, with changes to the way heart beats, the digestive symptom works.
I didn’t know that cancer surgery might include a hysterectomy and removing some or several organs, lymph nodes and body parts I’d never heard of. I didn’t know how it’s impossible to know what is from cancer, chemo, menopause or the piles of pills one is prescribed.
I didn’t know how much the body can endure and still keep going. I didn’t know I’d have a body that would have to learn and know all that I was mostly ignorant about -even though cancer is a disease not unknown to my own family members.
I am still learning and knowing and going. I hope what I learn keeps others from having to have first-hand knowledge of the cancer experience.
And even as I say that I know the ways I’ve been changed are not all bad, hard, or grueling.
I didn’t know that at, even in the midst of being consumed by all things basic bodily functioning (breathing, heart beating, eating, pooping, sleeping, and staying alive), one can also be grateful, satisfied, and appreciate life and loved ones.
I know it now and feel grateful daily.
Five months after my diagnosis, I’m what’s called NED (No Evident Disease). It means that after surgery, and then 5 rounds of chemo, a carbo/taxol combination every 3 weeks, there is no sign of ovarian cancer. My CA 125, a cancer marker in the blood, is back to normal. Things are looking better today and I’m grateful, optimistic, relieved, but also know that my life is forever changed, and I’ll never be out of the woods.
Despite my NED status, my chances of being alive in 10 years are 15%.
Despite my NED status, my chances of being alive in five years are less than 30%.
Did you know 70% of those with ovarian cancer die within five years of being diagnosed?
I’m not a statistic, but a person – still, it’s hard not to do the calculations.
5 years from my diagnosis I’ll be 57, and my daughter 21.
5 years from my diagnosis, my partner will be 62.
Will we get to retire together, ever? Will I get 5 years?
It’s hard not to wonder if some or all of those five years are what most would consider “good” years and how I will manage well no matter what? And how my loved ones will fare…
So I focus on moments, days, and now.
My new mantra remains, “In this moment….”
It’s how I approach all of my days.
I do think and worry about the future, and even plan for the worst while also planning for the best. Because the best is always possible.
What if, I’m the 15% and live for 10 or more years? What if I make it to 62? What if a new way to detect, manage, or treat ovarian cancer is discovered? What if I discover some synergy in remedies and medicines not yet combined?
Maybe I will see my kid graduate college or start a career. Maybe I’ll help her shop for furniture in a new apartment. No one knows the future. No one guaranteed more than now.
Maybe I’ll get to go to Europe with my partner, elope and return married, or stay forever engaged.
Maybe I’ll attend a mother-daughter yoga retreat with friends like I’ve always wanted to do.
Maybe I’ll spend a month at a cabin writing and eating good food with my besties?
Maybe I’ll be able to be there for my family members and friends the way they have been there for me?
Maybe I’ll get to walk my dog at the same beach and park, with my guy, my brother and sister-in-law, and our dogs and kids?
I don’t know how much time I’ll get or what life holds.
I know when my Nana died in her mid 60’s it seemed way too soon. I know that now, if I make it to my mid 60’s, it will be miraculous.
I don’t put as much into my retirement savings.
I think more about how to spend time, and money, now.
These are not negative thoughts they are the thoughts of someone contending with cancer and wide awake while pondering my own mortality.
“You won’t die of this,” some have said. “Cancer won’t kill you.”
But no one knows that for sure. It’s not an assurance the oncologists offer.
People mean well when they say such things but I no longer bite my tongue when I hear these words.
I say, “I might die of this,” (and I think, but don’t say, and you may as well).
I do remind people that we are all going to die and few of us will get to choose the time or place or method. It’s not wrong to acknowledge mortality. It’s not depressing and it does not mean one is giving up. I want to be responsible, and quickly, as I don’t have the luxury to be as reflective as I used to be because cancer is all-consuming.
I’ve barely had a moment to reflect on the past five months never mind the last five decades. I am trying to stay on top of the bare minimum requirements of being alive. I can’t yet keep up with emails or phone calls or visits. Projects and goals and plans of all kinds have shifted, paused, halted, or been abandoned.
My energy is now a resource I have to monitor and preserve. My will is not something I can endlessly tap into or call upon to motor me and keep me motivated. There’s no resource I have yet to tap into or call upon. Each day, I must consciously and repeatedly work to fill the well. And now, when friends and family who work while sick, I no longer think they are tough or strong. I think of how we routinely punish and ignore our bodies. I notice how often we run on fumes, require more of ourselves than we have as though we will never tire out.
I think of all those who must or feel they must keep going no matter what, without pause or rest, oblivious to the toll it will take or of those who have systems that can’t fight their germs. And I think of employers who sometimes require it because they offer no paid time off.
I used to run myself ragged. I used to say, “I’m digging deep, into my bone marrow if I have to.” I wasn’t being literal.
Now, when my iron and my platelets go low, I think of my old words in new ways. Now, even my bone marrow isn’t what is used to be.
I’m entirely who I always was and completely different.
It’s both.
I am more and less of who I was.
My life and days are simple and structured now and also heavy, layered, and complex. Who and what fills my day, by choice and not by choice, is radically different.
Cancer changed my life. That’s irrefutable and will be whether I live or die in the sooner or in the later.
I speak with and interact with doctors, nurses, life insurance and disability insurance and pharmacists more. I spend more money on supplements, clean eating, and make more time to walk, exercise, and sleep. There’s so much less I am capable of.
But sometimes, even without hair, I feel totally like myself.
Sometimes, like this week, my daughter caught me in the middle of life, reading a book, petting the cat, on my bed in my heated infrared sauna blanket. I was relaxed and at ease.
I shared this photo and someone commented on how my “cat scan” was quite feline, – the image brought a whole new meaning to the “cat scan” image.
I laughed and laughed and laughed. I’m still laughing.
In this moment, in many moments, I’m humbled by the enormity of all things cancer and being alive. That’s real. That’s there. It can be intense.
But also, in this moment, I’m laughing.
And laughing, it turns out, is my favorite way to live.

When not recovering or coping with her recent ovarian cancer diagnosis, chemo brain, and the other treatment-related side effects, Christine “Cissy” White works as Community Manager of the Parenting with ACEs community on ACEs Connection and blogs at www.healwritenow.com. White has been published in The Boston Globe, Spirituality and Health, Ms. Magazine, The Mighty, To Write Love on Her Arms, Elephant Journal, the Center for Health Journalism, and ACEs Too High. She is the 2019 recipient of the Touching Trauma at Its Heart Award, given by the Attachment Trauma Network for her work advocating on behalf of families coping with traumatic stress from developmental trauma. White has led Parenting with ACEs, Parenting After Trauma, and Writing to Heal workshops and speaks passionately about the need for first-person perspectives and the power of lived expertise. Her survivor-led advocacy has been written about in The Atlantic, Huffington Post, and The Mighty.
Today, we’re extremely proud to introduce our first-ever Empowered! podcast. Empowered! will bring you conversations around topics that are important to patients and care partners.
For our first episode, we meet Andrea Conners. Andrea is Patient Empowerment Network’s Executive Director. Andrea shares a little bit about herself, about PEN, and her inspiration in getting involved.